Syringomyelia is a disorder in which a fluid-filled cyst/syrinx forms within the spinal cord. It is progressive, meaning that the cyst grows with time causing compression and damage to the spinal cord. The cyst usually begins in the neck/cervical spine but can develop in any area along the spinal cord. There are several possible causes; however, most are associated with a condition known as Chiari malformation. This is where the skull and neck come together, and either the skull is too small or shaped in a way that causes brain tissue to come out and settle in the spinal canal.
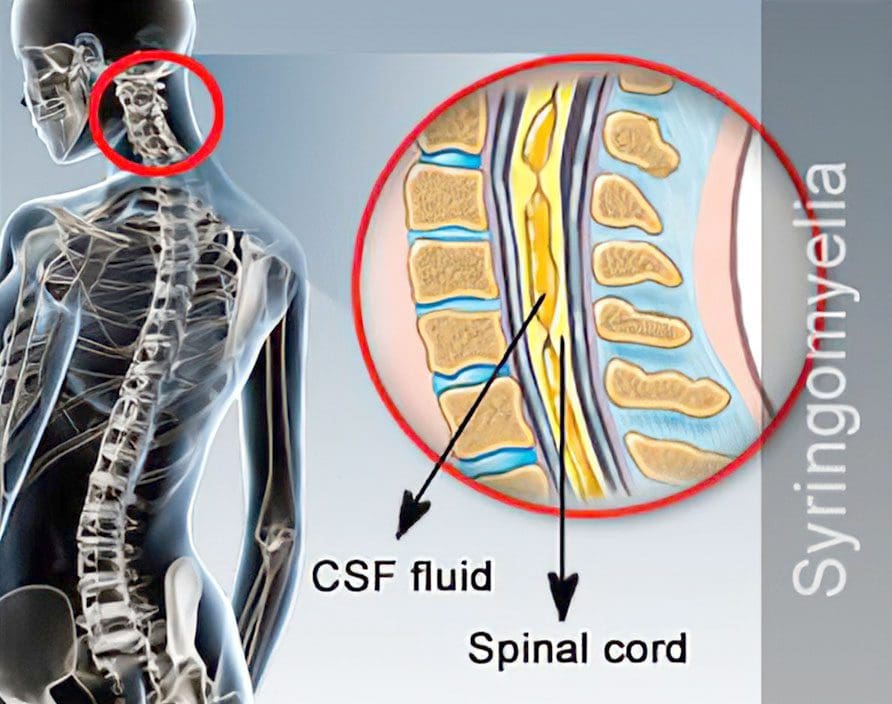
Syringomyelia Causes
Syringomyelia can be caused by or from complications of:
- Congenital disabilities like Chiari malformation
- Chiari type I malformation develops during the fetal developmental stage and causes the lower part of the brain or cerebellum to stick out from its standard location.
- Hemorrhage/bleeding
- Inflammation of the spinal cord from virus or bacterial infection like meningitis
- Spinal cord injury
- Spinal cord tumor
Symptoms
A damaged spinal cord disrupts communication between the brain and the body. Symptoms differ for every individual, but common syringomyelia symptoms include:
- Pain, stiffness, or weakness in the neck, arms, back, and/or legs
- Progressive numbness
- Headache/s
- Sensitivity to heat and cold
- Muscle atrophy, contractions, spasticity/tightness
- Skin rash
Symptoms usually develop slowly, but exercise, coughing, or some form of strain can cause sudden onset.
Diagnosis
Physical and neurological exams are performed to determine loss of feeling or inability to move around normally, like walking. Diagnostic tests of the spine will include a CT scan with contrast dye and/or an MRI. Early detection can help before it progresses, causing further damage, and delaying treatment can cause irreversible spinal cord injury. It is recommended at the first sign of symptoms to contact a doctor.
Treatment
Some individuals who have syringomyelia may have no symptoms. These individuals can go about their everyday lives but are recommended to be cautious with neck and back strain. For individuals experiencing symptoms, the primary treatment objectives are to:
- Stop or control damage to the spinal cord
- Preserve function
- Prevent disability
- Treatment options include:
- Draining the cyst
- Surgical removal of the cyst
- Chiropractic and physical therapy could be included in the treatment plan to help the individual rebuild lost muscle strength and regain flexibility.
All too often, individuals with this disorder experience treatment delay/s because symptoms can be nonspecific or vague. Education is the key, and individuals can be diagnosed sooner by paying attention to the body's warning signs.
Body Composition
Does too much protein hurt the kidneys?
While protein restriction can be appropriate for treating existing kidney disease, research shows that high protein intake in healthy individuals does not disrupt or cause damage to the kidneys or kidney function. The amino acids in protein are more likely to be excreted through urine when not being used. However, there are certain risks associated with consuming too much protein, and it is recommended to keep track of protein intake. Eating more protein:
- Makes the body feel full longer
- Can help curb overeating
- Is essential for recovery and growth
When achieving daily caloric goals, maintaining a balance of nutrients like carbohydrates and healthy fats is essential for overall health.
The information herein is not intended to replace a
one-on-one relationship with a qualified health care professional, licensed
physician, and is not medical advice. We encourage you to make your own health
care decisions based on your research and partnership with a qualified health
care professional. Our information scope is limited to
chiropractic, musculoskeletal, physical medicines, wellness, sensitive health
issues, functional medicine articles, topics, and discussions. We provide and
present clinical collaboration with specialists from a wide array of
disciplines. Each specialist is governed by their professional scope of
practice and their jurisdiction of licensure. We use functional health &
wellness protocols to treat and support care for the injuries or disorders of
the musculoskeletal system. Our videos, posts, topics, subjects, and insights
cover clinical matters, issues, and topics that relate to and support, directly
or indirectly, our clinical scope of practice.* Our office has made a reasonable
attempt to provide supportive citations and has identified the relevant
research study or studies supporting our posts. We
provide copies of supporting research studies available to regulatory boards
and the public upon request.
We understand that we cover matters that require an
additional explanation of how it may assist in a particular care plan or
treatment protocol; therefore, to further discuss the subject matter above,
please feel free to ask Dr. Alex
Jimenez or contact us at 915-850-0900.
Dr.
Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN*
email: coach@elpasofunctionalmedicine.com
Licensed in: Texas & New Mexico*
References
Batzdorf, Ulrich. "Primary spinal syringomyelia. Invited submission from the joint section meeting on disorders of the spine and peripheral nerves, March 2005." Journal of neurosurgery. Spine vol. 3,6 (2005): 429-35. doi:10.3171/spi.2005.3.6.0429
Di Lorenzo, N, and F Cacciola. "Adult syringomyelia. Classification, pathogenesis and therapeutic approaches." Journal of neurosurgical sciences vol. 49,3 (2005): 65-72.
Fernández, Alfredo Avellaneda et al. "Malformations of the craniocervical junction (Chiari type I and syringomyelia: classification, diagnosis, and treatment)." BMC musculoskeletal disorders vol. 10 Suppl 1, Suppl 1 S1. 17 Dec. 2009, doi:10.1186/1471-2474-10-S1-S1
Naftel, Robert P et al. "Worsening or development of syringomyelia following Chiari I decompression: case report." Journal of neurosurgery. Pediatrics vol. 12,4 (2013): 351-6. doi:10.3171/2013.7.PEDS12522
Roy, Anil K et al. "Idiopathic syringomyelia: retrospective case series, comprehensive review, and update on management." Neurosurgical focus vol. 31,6 (2011): E15. doi:10.3171/2011.9.FOCUS11198




