El Paso, TX. Chiropractor, Dr. Alexander Jimenez focuses on degenerative and demyelinating diseases of the nervous system, their symptoms, causes and treatment.
Degenerative & Demyelinating Diseases
Motor Neuron Diseases
- Motor weakness without sensory changes
- Amyotrophic lateral sclerosis (ALS)
- ALS Variants
- Primary lateral sclerosis
- Progressive bulbar palsy
- Inherited conditions that cause anterior horn cell degeneration
- Werdnig-Hoffmann disease in infants
- Kugelberg-Welander disease in children and young adults
Amyotrophic Lateral Sclerosis (ALS)
- Affects patients 40-60 years of age
- Damage to:
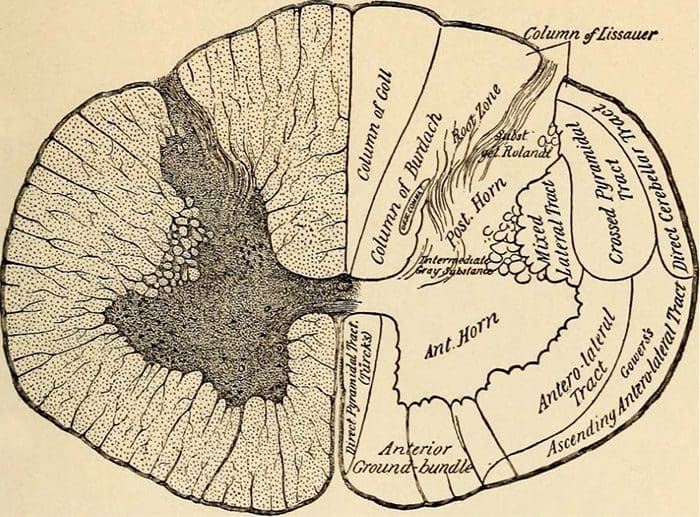
- Anterior horn cells
- Cranial nerve motor nuclei
- Corticobulbar and corticospinal tracts
- Lower motor neuron findings (atrophy, fasciculations) AND upper motor neuron findings (spasticity, hyperreflexia)
- Survival ~three years
- Death results from weakness of the bulbar and respiratory musculature and resultant superimposed infection
ALS Variants
- Usually eventually evolve into typical ALS pattern
- Primary Lateral Sclerosis
- Upper motor neuron signs begin first, but patients do eventually have lower motor neuron signs as well
- Survival can be ten years or longer
- Progressive Bulbar Palsy
- Selectively involves the head and neck musculature
Inherited Motor Neuron Conditions
- Anterior horn cell degeneration
- Werdnig-Hoffmann disease
- Affects infants
- Kugelberg-Welander disease
- Affects children and young adults
Church, Archibald. Nervous and Mental Diseases. W.B. Saunders Co., 1923.
Alzheimer Disease
- Characterized by neurofibrillary tangles (aggregates of hyperphosphorylated tau protein) & beta-amyloid plaques
- Generally occurring after age 65
- Hereditary risk factors
- Mutations in the beta amyloid gene
- Epsilon 4 version of apolipoprotein
Diagnosis
- Pathologic diagnosis is the only way to definitively diagnose the condition
- Imaging may be able to rule out other causes of dementia
- Functional imaging studies may be further developed to become diagnostically useful in the future
- CSF studies examining for tau proteins and beta amyloid may become useful as diagnostic tests in the future
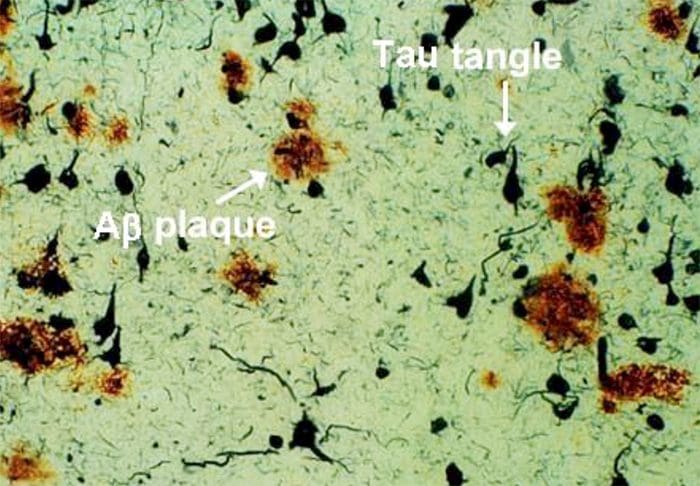
Amyloid Plaques & Neurofibrillary Tangles
http://sage.buckinstitute.org/wp-content/uploads/2015/01/plaque-tanglesRNO.jpg
Brain Areas Affected by Alzheimer Disease
Hippocampus
- Loss of recent memory
Posterior temporo-parietal association area
- Mild anomia & constructional apraxia
Nucleus basalis of Meynert (cholinergic neurons)
- Changes in visual perception
Progression
- As more and more cortical areas become involved, the patient will develop more severe cognitive deficits, however paresis, sensory loss, or visual field defects are features.
Treatment Options
Medications that inhibit central nervous system acetylcholinesterase
- Donepezil
- Galantamine
- Rivastigmine
Aerobic Exercise, 30 minutes daily
PT/OT care to maintain activities of daily living
- Antioxidant and anti-inflammatory therapies
- In advanced stages, may require full time, in home care
Vascular Dementia
- Cerebral arteriosclerosis leading to stroke
- Patient will have documented stroke history or signs of prior stroke (spasticity, paresis, pseudobulbar palsies, aphasia)
- May be associated with Alzheimer Disease if due to amyloid angiopathy
Frontotemporal Dementia (Pick’s Disease)
Familial
Affects the frontal and temporal lobes
- May be seen on imaging if advanced degeneration in these areas
Symptoms
- Apathy
Disordered behavior
- Agitation
- Socially inappropriate behavior
- Impulsivity
Language difficulties
Generally no memory or spatial difficulties
Pathology reveals Pick bodies within the neurons
Results in death in 2-10 years
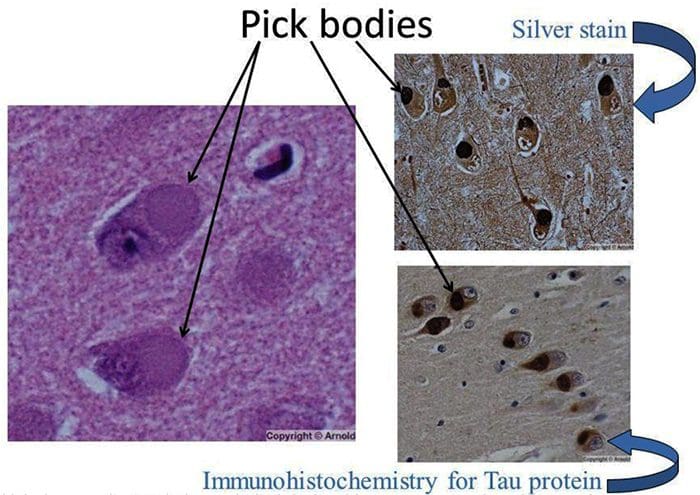
Pick Bodies/Cytoplasmic Inclusions
http://slideplayer.com/9467158/29/images/57/Pick+bodies+Silver+stain+Immunohistochemistry+for+Tau+protein.jpg
Treatment
Antidepressants
- Sertraline
- Citalopram
Discontinue medications that can cause memory impairment or confusion
- Sedatives
- Benzodiazepines
Exercise
- Lifestyle modification
- Behavioral modification therapy
Parkinson Disease
May occur at any age, but rare before age 30, and increases prevalence increases in older populations
Familial tendency but can also without family history
Can be induced by certain environmental factors
- Exposure 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP)
- Compounds which produce excessive free radicals
Affects substantia nigra pars compacta
- Dopaminergic neurons
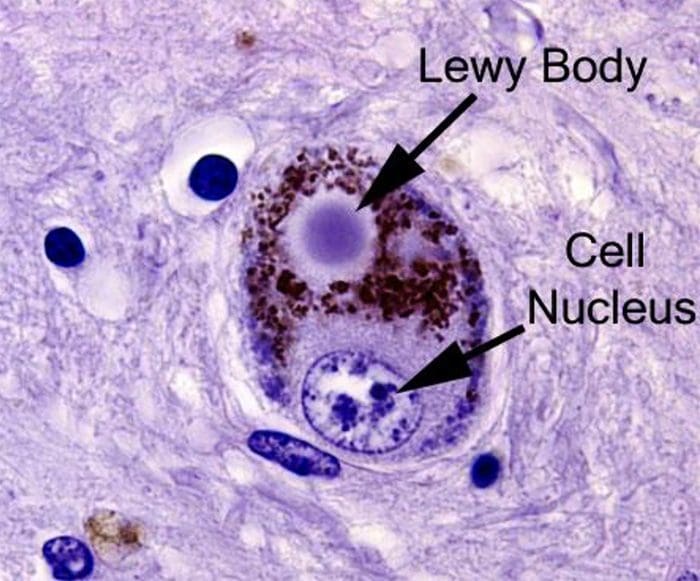
On pathology, the presence of Lewy Bodies
- Accumulation of alpha-synuclein
Lewy Bodies
https://scienceofpd.files.wordpress.com/2017/05/9-lb2.jpg
Symptoms of Parkinsonism
Rigidity (all planes)
- Passive ROM
- Active movement
- May be of cogwheel nature due to tremor symptoms
Bradykinesia
- Slowness of movement
- Inability to initiate movement
- Freezing
Resting tremor (“pill-rolling”)
- Created by oscillation of opposing muscle groups
Postural defects
- Anteriorly flexed (stooped) posture
- Inability to compensate for perturbations, resulting in retropulsion
Mask-like facies
Mild to moderate dementia
- Later in progression, due to lewy body accumulation
Pathology
Deficiency of dopamine in the striatum (caudate and putamen) of the basal ganglia
Dopamine normally has the effect of stimulating the direct circuit through the basal ganglia, while inhibiting the indirect pathway
Carbidopa/Levodopa
Most common treatment is a combination drug
Levodopa
- A dopamine precursor that crosses the blood-brain barrier
Carbidopa
- Dopamine decarboxylase inhibitor that does not cross the BBB
- Amino acids will reduce effectiveness (competition) and so medication should be taken away from protein
Prolonged Treatment With Carbidopa/Levodopa
The patient’s capacity to store dopamine declines with medication use and therefore the improvements from the medications will last for shorter and shorter periods the longer the medication is used
Over time can result in proliferation of dopamine receptors
- Peak-dose dyskinesia
Long term use puts stress on the liver
Other side effects can include nausea, hypotension and hallucinations
Other Treatment Options
Medications
- Anticholinergics
- Dopamine agonists
- Dopanime breakdown inhibitors (Monoamine oxidase or catechol-O-methyl transferase inhibitors)
- High dose glutathione
Brain balancing functional neuro-rehab exercises
- Vibration
- Retropulsive stimulation
- Repeated reflex stimulation
- Targeted CMT/OMT
Multiple System Atrophy
Symptoms of Parkinson Disease paired with one or more of the following:
- Pyramidal signs (Striatonigral degeneration)
- Autonomic dysfunction (ShyDrager syndrome)
- Cerebellar finding (Olivopontocerebellar atrophy)
Generally not responsive to standard Parkinson Disease treatments
Progressive Supranuclear Palsy
Fast progressing degeneration involving tau proteins in many areas including the rostral midbrain
Symptoms usually start around ages 50-60
Gait difficulty
Significant dysarthria
Voluntary vertical gaze difficulty
Retrocollis (dystonic extension of the neck)
Severe dysphagia
Emotional lability
Personality changes
Cognitive difficulty
Does not respond well to standard PD treatment
Diffuse Lewy Body Disease
- Progressive dementia
- Severe hallucinations and possible paranoid delusions
- Confusion
- Parkinsonian symptoms
Multiple Sclerosis
Multiple white matter lesions (plaques of demyelination) in the CNS
- Variable in size
- Well-circumscribed
- Visible on MRI
Optic nerve lesions are common
Peripheral nerves are not involved
Uncommon in children under 10, but usually presents before age 55
Viral infection may trigger an inappropriate immune response with antibodies to a common virus-myelin antigen
Infectious and immune mechanisms contribute
Types Of MS
Primary progressive MS (PPMS)
Secondary progressive MS (SPMS)
Relapsingremitting multiple sclerasis (RRMS)
- Most common type
- Can develop acutely, spontaneous appear to resolve and return
- Eventually becomes like SPMS
Optic Nerve Involvement
In 40% of MS cases
Pain with eye movements
Visual field defect (central or paracentral scotoma)
Funduscopic examination
- May reveal papilledema if the plaque involves the optic disk
- May not appear unusual if plaques are behind the optic disk (retrobulbar neuritis)
Medial Longitudinal Fasciculus Involvement
Demyelination of the MLF results in internuclear ophthalmoplegia
- During lateral gaze there is paresis of the medial rectus and nystagmus of the contralateral eye
Convergence remains normal
Other Possible MS Symptoms
Myelopathy
- Spastic hemiparesis
- Impaired sensory tracts (DC-ML)
- Paresthesias
Cerebellar involvement
- Ataxia
- Dysarthria
Vestibular system involvement
- Imbalance
- Mild vertigo
- Nystagmus
Tic douloureux (trigeminal neuralgia)
Lhermitte's symptom
- Shooting or tingling sensation referred to the trunk and limbs during neck flexion
- Fatigue
- Hot bath often exacerbates symptoms
Differentials To Consider
Multiple emboli and vasculitis
- May appear as white matter damage on MRI
Central nervous system sarcoidosis
- Can produce reversible optic neuritis and other CNS signs
Whipple disease
- Inflammatory lesions
- Usual eye movements
Vitamin B12 deficiency
- Dementia
- Spasticity
- Dorsal column
Meningovascular syphilis
- Multifocal CNS damage
CNS Lyme disease
- Multifocal disease
Differential Diagnosis: Diagnostic Studies
Blood tests can help to distinguish
- Complete blood count
- Antinuclear antibodies (ANA)
- Serum test for syphilis (RPR, VDRL, etc.)
- Fluorescent treponemal antibody test
- Lyme titer
- ESR
- Angiotensin converting enzyme level (to r/o sarcoidosis)
Diagnostic Studies Of MS
MRI with and without contrast
- 90% of MS cases have detectable MRI findings
CSF findings
- Elevation of mononuclear white blood cells
- Oligoclonal IgG bands
Increased globulin to albumin ratio
- This is also seen in 90% of MS cases
Increased myelin basic protein levels
Prognosis
- Average survival after diagnosis is ~ 15 to 20 year
- Death is usually from superimposed infection and not due to the effects of the disease itself
Sources
Alexander G. Reeves, A. & Swenson, R. Disorders of the Nervous System. Dartmouth, 2004.Swenson, R. Degenerative Diseases of the Nervous System. 2010.