Chiropractic scientist, Dr. Alexander Jimenez appears at the most common injuries incurred from the first team game in the modern-day Olympics...
Water polo, while not played with the ancients, was the first team sport played in the Olympics, beginning at the 1900 games in Paris. The prevalence of water polo grew, in part, due to the reckless, almost violent, style. The body or pool of water became a coliseum of sorts. Today, this degree of play still exists. In a survey of injury incidence performed by the Federation International de Natation Amateur (FINA) throughout the 2004 and 2008 Olympic Games and the 2009 FINA World Championships, water polo was found to possess the highest incidence of accidents, the many traumatic accidents, and also the most time lost from play due to injuries(1).
Central Control
Most water polo injuries occur to the head. FINA reports that 56% of all injuries suffered by water polo athletes in the 2004 Olympic games have been to the head(two). Arms vie to get a ball that can be thrown at speeds of up to 70 km per hour by women, and faster than that by guys; and the head is an easy target for both(3).Lacerations to the mind can normally be tended to poolside, unless they involve the cornea of the eye. Corneal abrasions can be painful and serious. Remove from the game, dissuade him from rubbing against the eye if corneal abrasion is suspected and refer to a doctor. Medication to prevent disease, calm inflammation and decrease pain may be prescribed.
Blows to the head or face, either from another player or from the ball , can break delicate bones, impacting eyes and sinuses. In these cases, seek prompt medical attention for the athlete and evaluate for signs of traumatic brain injury. Trainers must rely on other players to attract the player poolside if the player looses consciousness in the sport. All teams must periodically conduct drills that are life-saving so that players are ready to save yet another, if the situation arise. In a poll comparing team sports in the 2004 Olympic Games at Athens, water polo was discovered to possess the best variety of head injuries(2). Water polo teams, the same as the rest of the sport teams, should have head injury protocols such as baseline testing and return to perform. Water polo generally falls under aquatics programming rather than field sports. Thus, head-injury protocols may be lacking. Returning to combat may appear epic, before cleared by a physician, but it's better to err on the side of retreat and caution.
The only protective equipment a water polo athlete wears is over the ears. This protects the eardrum and also lessens the trauma. Despite the covering, traumatic rupture of the eardrum is common and generally occurs when struck or kicked while under water. The increased pressure in the ear canal tears a hole in the tympanic membrane. Ruptured eardrums heal in about three months they need to be kept dry throughout the healing process. This usually means no pool time unless your doctor approves of using a earplug and swim cap.
Another ear disease that keeps a water polo athlete is otitis externa. It's a disease in the external auditory canal. The auditory canal becomes an ideal host to get a proliferation of germs if it isn't dried well, loses much of ear wax, or the cerumen, or suffers a cut. No matter the origin, the result is a very debilitating condition that often comes on suddenly and quickly.
Ear drops that usually include an antibiotic, antifungal, and steroid suspended in an solution to normalize the pH of the canal are involved by treatment for otitis externa. During treatment, athletes should continue to keep the ear dry and remain out of their water. Downtime may be a week or longer, thus avoidance is more preferable. An earache can be prevented by routine hygiene from side- lining a water borne warrior. The pH is normalized by a solution of one part rubbing alcohol to one part white vinegar when players get from the pool's usage and aids drying. Advise athletes to never add anything to wash them. Instead, dry ears with a hair dryer on the lowest setting, held a foot away in the ear.
Surveillance & Reconnaissance
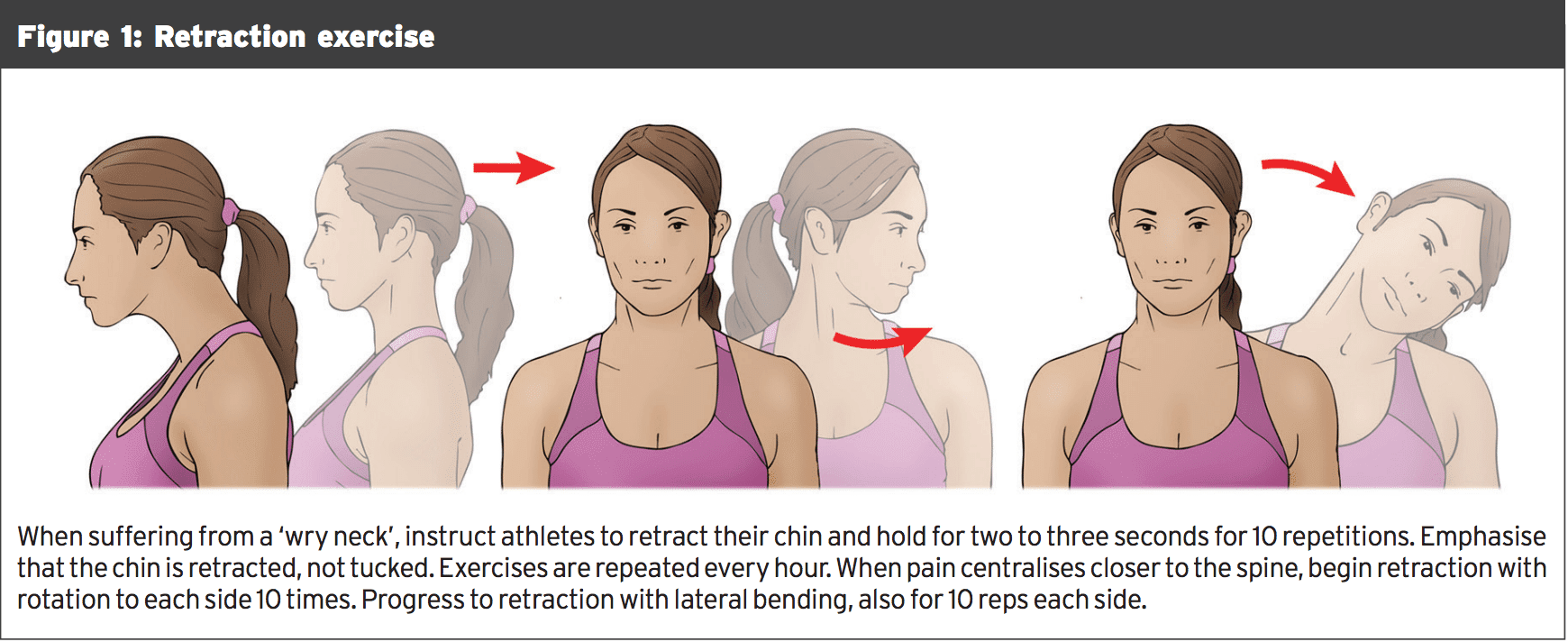
The water polo athlete awakens with head out of the water so as to maintain a visual on his competitions and the ball. This posture requires activation of the posterior and lateral neck muscles, which can go into spasm, causing a 'wry neck' or a 'crick' . The pain appears suddenly with a head turn, or comes on at the morning after 'sleeping wrong'. The pain limits motion of the throat and some- times the shoulder. Treatment for a 'wry neck' includes physiotherapy , medication for pain, and ice. Retraction exercises are especially effective but have to be repeated hourly before pain and motion improve, usually over a few days (see Figure 1).Intrigue
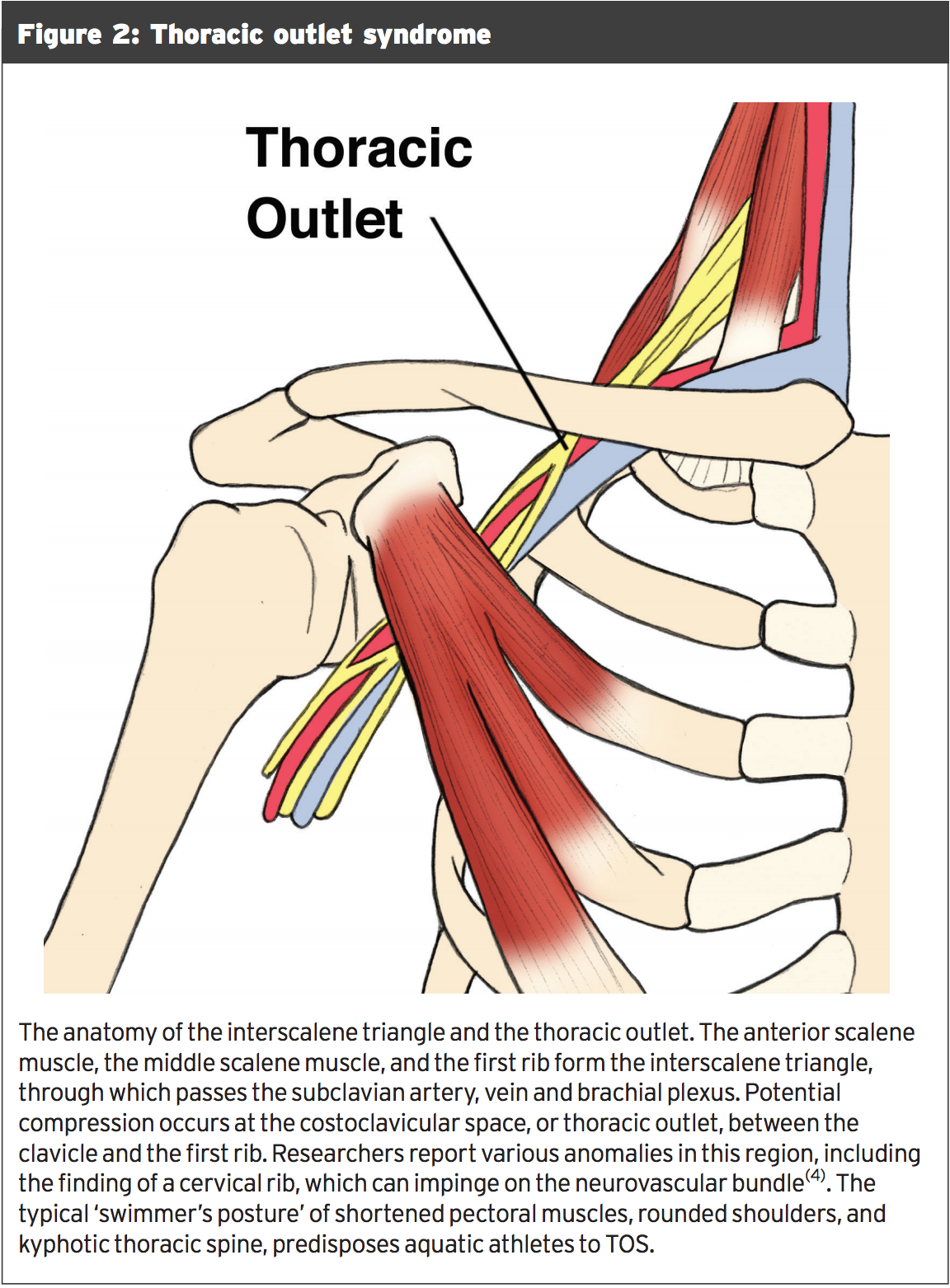
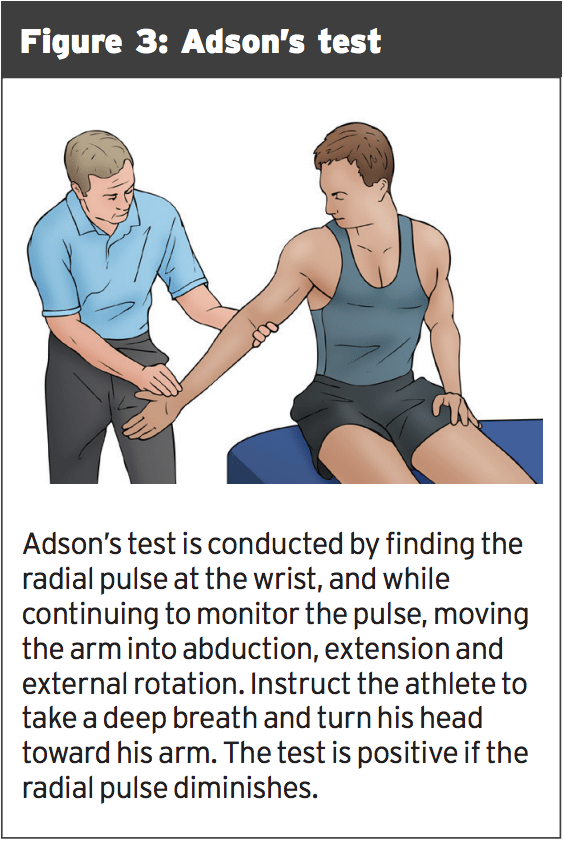
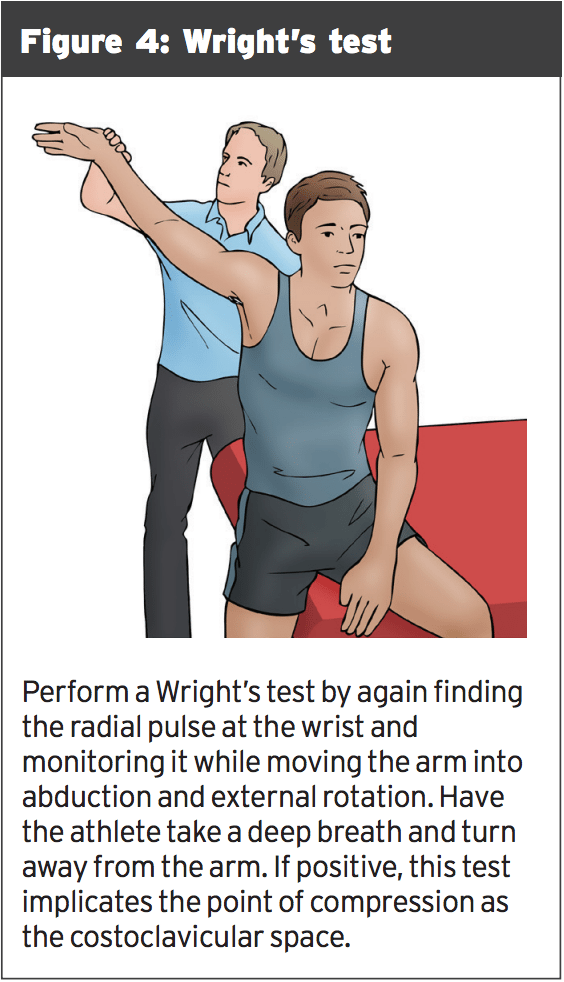
A master of lies and deception, thoracic outlet syndrome (TOS) causes pain in the shoulder at the extremes of abduction and external rotation (a position assumed in water while both swimming and throwing) just as shoulder joint injuries do. But with TOS, the pain is a result of compression of the neurovascular bundle that moves through the interscalene triangle and the thoracic outlet, not in any pathology inside the shoulder (see Figure 2). Athletes with TOS might have difficulty throwing the ball because of weakness of hand muscles, or senses of coolness or tingling along the arm or hand, holding, and grabbing. It may be difficult to keep fingers together during the pull phase of the stroke, when swimming. There is absolutely no instability; nonetheless, be cautious as shoulder pathology and TOS can exist concurrently.The 'armory'
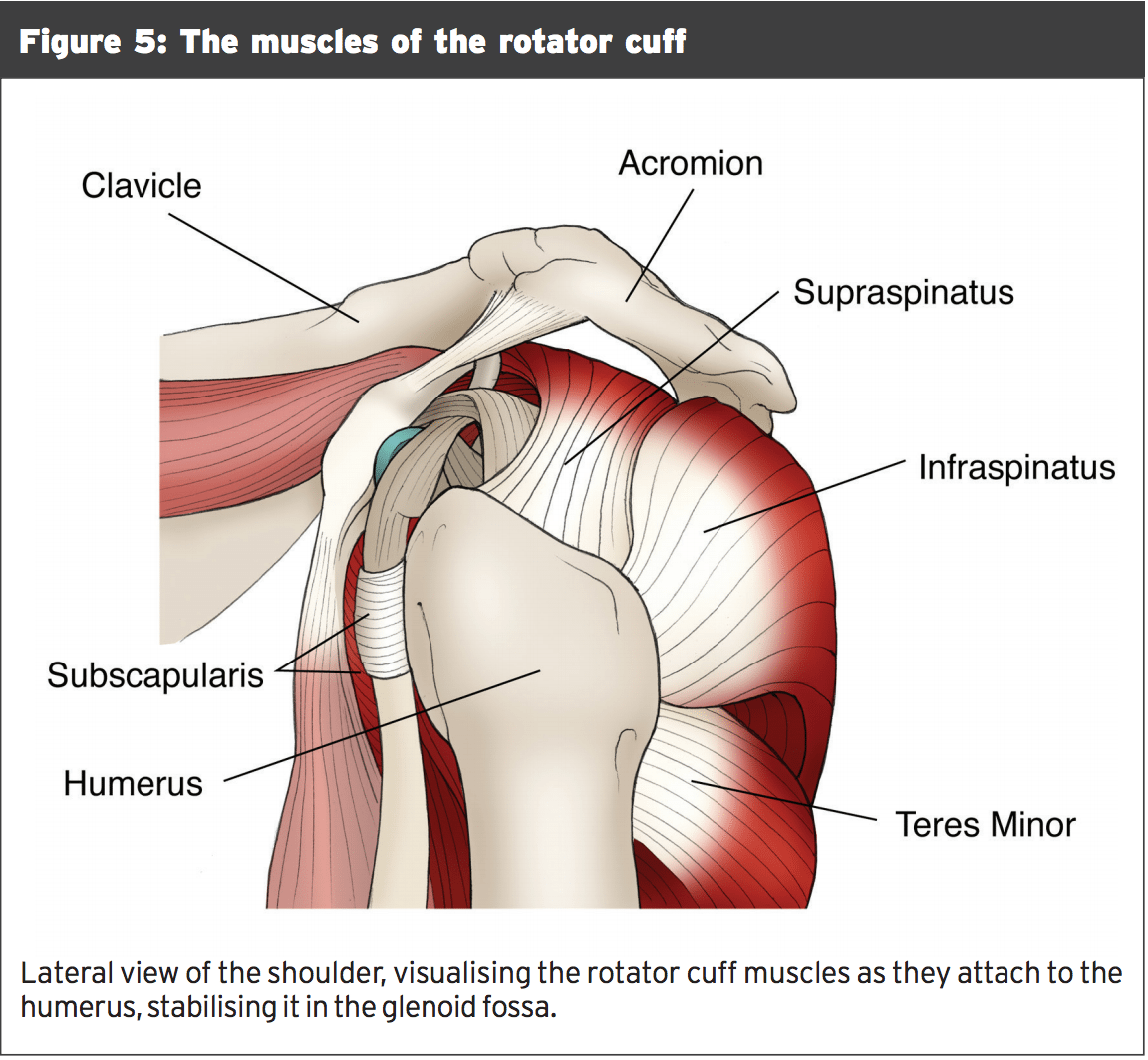
Up to 80% of water polo players complain of a painful shoulder, and the incidence increases with the level of play(5). Water Resistant athletes are at risk for shoulder injury, being over and swimmers- mind throwers. The overhand throw is similar but without the help of a base of support. Hence, the back moves as one device, minus the segmented spinning in a baseball throw, contributing only 30 percent to 35 percent of the rate generating force acted upon the ball ; and departing the shoulder to provide the rest(5,6).The muscles of the rotator cuff, the supraspinatus, the infraspinatus, the teres minor, and the subscapularis (SITS), are responsible for stabilizing the humerus within the shallow glenoid fossa, gloomy the humerus throughout shoulder movement, and for both internal and external shoulder rotation (see Figure 5). These muscles fatigue more quickly in water polo due to increased activation at the head-up swimming posture when compared to freestyle(5). When the muscles are stressed, due to overuse, improper procedure, or muscle imbalances, hypoxia, which results in cell death or apoptosis is experienced by them. Early cell death inside the tendon, termed but commonly referred to is treated with eccentric strengthening, remainder, and proper technique. Too much stress, along with the fascia may rupture and degenerates beyond repair. It's very important to track any complaints of shoulder pain so that pressure into the muscles may be treated while the injury is still minor.
Posterior shoulder dislocation or acromioclavicular dislocations (also known as AC separations) occur in the guardian that blocks the shot's arm with his straight arm (shoulder flexed, elbow extended). The shot's arm compels the humerus and pushes against the shield's arm backward. Within an AC separation, the defender's arm is driven inferiorly and posteriorly. The scapula is thrust posteriorly but the ribs stop the clavicle. The joint between the scapula and the clavicle separates, and with sufficient force the clavicle could break.
A general name for shoulder impingement syndrome that is joint, swimmer's shoulder, plagues water polo athletes. They lose their ability to depress the head as it goes causing it to migrate up toward the acromion. The shoulder mechanisms that are place the bursa if quite lax and joint capsule itself -- for getting caught between those constructions at risk. The restoration of shoulder mechanisms through strengthening the shoulder stabilizers and using proper swimming technique prevents the constructions that are impinged from ripping and relieves the pain.
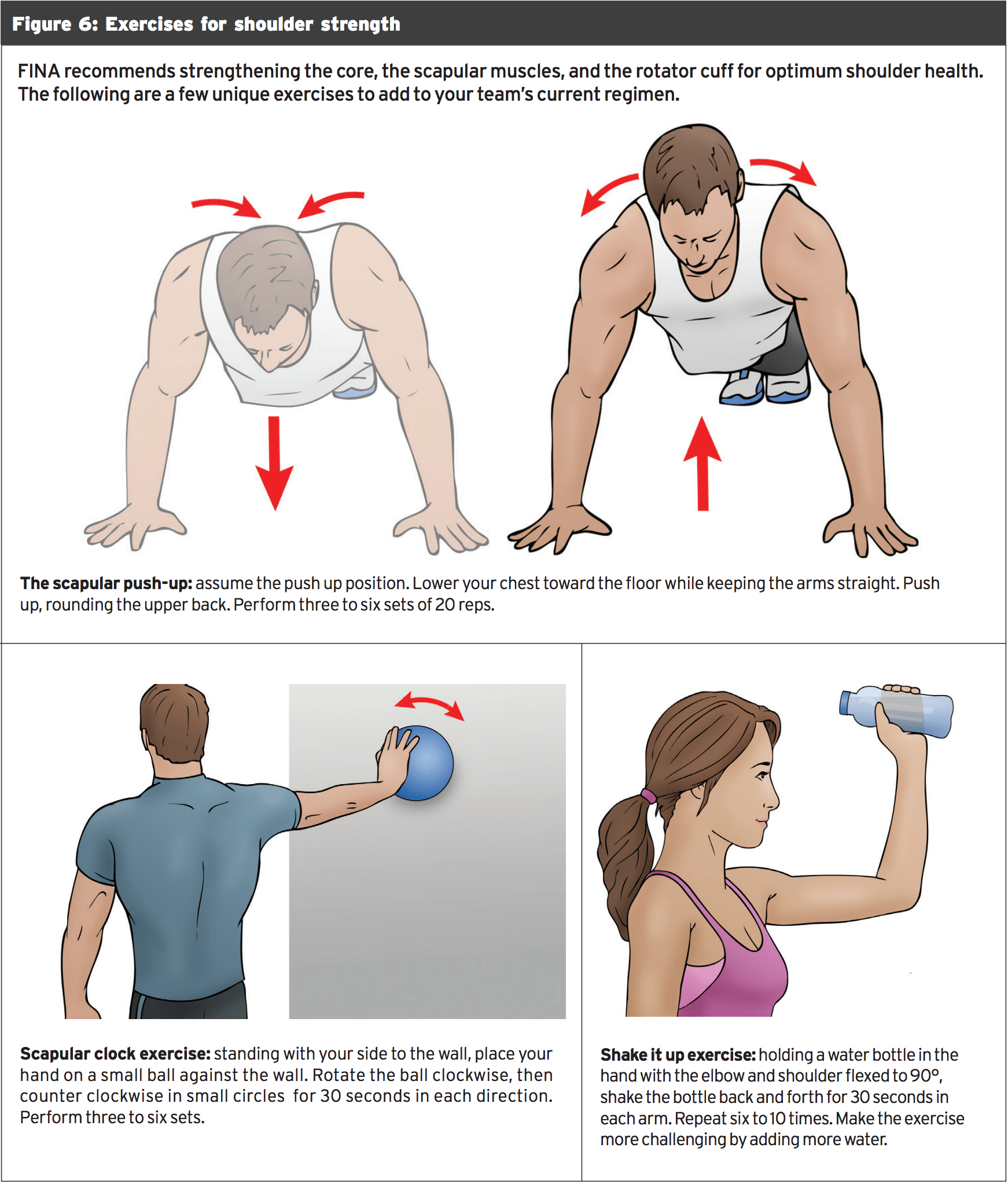
Seeing as the arsenal for propulsion and lies from the shoulder, it is a fantastic idea to maintain shoulder health through a targeted strengthening program. Endure the collective groan because they tire of exercising the unsexy and exhausted shoulder of your team. It helps maintain your front line in the water, along with the reserves ready for action (see Figure 6).
Maintaining The Barrage
The only way to score in water polo is to throw the ball in the target -- and water polo athletes do of projecting lots and lots. Without the benefit of a base of support, the water polo athlete must generate the vast majority of the power to your throw from the arm. The throwing, rather than the swimming, causes elbow injuries.The ulnar collateral ligament (UCL) joins the humerus using the ulna medially and provides the vast majority of valgus stability to the elbow (see Figure 7). It fails with loads over 260 N(4). The forces generated through the water polo throw often exceed this, leading to micro tears into the ligament(5). Injury to the UCL produces pain over the medial elbow. Isolated UCL injuries respond to a conservative therapy of physiotherapy modalities, relaxation, and strengthening of muscles that are supporting. Acute ruptures require surgical fixation.
Symptoms of pain in the posterior- elbow, particularly in expansion improve with therapy. The use of taping to limit whole elbow extension or bracing enables play and relieves the strain. If symptoms persist, Surgical intervention is justified although infrequent.
Osteochondritis dissecans (OCD) can be probably brought on by the valgus stress at the elbow through throwing(7). OCD happens every time the subchondral bone is separated in by a sheet of cartilage on the capitulum. Athletes may complain of swelling and pain, accompanied by locking or grabbing at the joint. More common in the young, OCD can occur in adults with repetitive throwing. Researchers at Croatia also guess that untreated elbow hyperextension injuries, frequent in goalkeepers, may advance to OCD(7). Physical and physical therapy enable the separation to heal, but unresponsive cases require surgical fixation.
Hand To Hand Combat
Most of the accidents that occur to hand and the fingers are traumatic and severe. Battling over the chunk induces lacerations, fractures, and dislocations. The laceration that is most common is that a tear in the web space between two palms. Fix may be a simple closure of the wound or surgical intervention to reattach ligaments and torn tendons. Obtaining a force- can cause a hyperextension dislocation of a finger. Reduction is usually simple and the participant can perform with the finger 'buddy taped' if pain is controlled. A variety of fractures are treated with surgical or splinting pinning.Triumph
Although not battle, water polo is a competitive and demanding sport. The physicality of the sport means that accidents are often traumatic, and yet, the repetitiveness of this sport causes chronic injuries that are numerous . It is not uncommon for athletes to have battle scars. Keep the routine as healthy as possible through soil strengthening, and focus on throwing and swimming technique, which means that your team can ascend to the throne of victory.References
1. British journal of sports medicine 04/2011; 45(4):315.
2. The American Journal of Sports Medicine 05/2006; 34(4):565-76.
3. J Strength Cond Res. 2011 Nov;25(11):3051-8.
4. Croat Med J. 2007;48:281-8.
5. Alexander M, Hayward J, Honish, A. Water Polo: A Biomechanical Analysis of the Shot. Unpublished research report prepared for Water Polo Manitoba, The University of Manitoba, April, 2005.
6. Injury. 2013 Sep;44 Suppl 3:S46-8.
7. HSS J. Feb 2006; 2(1): 83–93.