Chiropractor, Dr. Alex Jimenez looks at also the dysfunctions — and also the gluteus medius and the way they are best rehabilitated…
Introduction
The Gluteus Medius (GMed) is a muscle that has received a substantial amount of interest amongst physical treatment world and the exercise fraternity. It’s a muscle that is often implicated in playing a role in stabilising the pelvis and controlling both the frontal, sagittal and coronal planes of motion of the lower limb. Dysfunction at the GMed has often been associated with a selection of pain syndromes including knee, knee, hip and back issues.Relevant Anatomy & Biomechanics
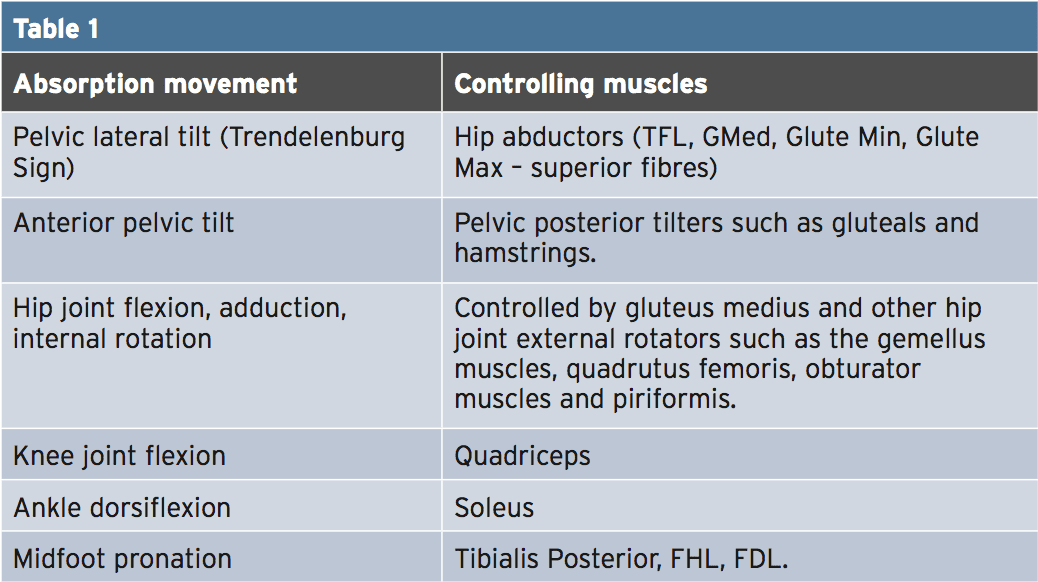
During weight bearing Movements such as posture period of walking/running, lunging, landing from a jump amongst others, the tendency for the lower limb joints is to absorb the effect of gravity. The force of gravity will create joint moments into certain instructions and muscles are required to work to counteract these forces (usually these muscles work isometrically and/or eccentrically). Table 1 explains the ‘absorbing’ muscles control these minutes that are joint and joint movments.The GMed is a hip muscle that is purported as among those muscles that regulates joint motion that subsequently controls limb kinetics that is lower round knee and the knee. The GMed will be described by anatomy textbooks as attaching to the crest and adding onto the greater trochanter. Its purpose is frequently described as being a hip abductor, hip the and rotator Pelvis on the femur during stance phase of gait. However, since Gottschalk et al (1989) indicate, its most important role may in fact be to compress the femoral head into the acetabulum during the stance phase of gait(9). The muscle is broken up anterior, middle and posterior.
The elements of the posterior portion run while the anterior and middle parts operate from the iliac crest to the anterosuperior aspect of the greater trochanter, almost parallel with the neck of the femur. The three parts of GMed Each have its nerve supply operating indicating that the muscular actions of the three heads are independent of each other.
Gottschalk et al (1989)(9) also ran EMG studies and they found that the GMed is not really that active in isolated abduction of the hip. This finding may well surprise readers, as it’s contrary to what has been taught for years in textbooks and human anatomy and biomechanics lectures. They observed that the tensor fascia lata (TFL) is significantly more active in isolated hip abduction. They went on to indicate that those GMed’s 3 heads have a phasic muscle activity. The posterior guided fibers are more active at heel strike, and the muscle gets recruited to anterior as motion occurs to posture of gait. To put it differently, the front portion of the muscle (which is anatomically similar to this TFL) is active at full posture and single-leg support phase, while the rear fibres fire strongly at initial heel strike.
Gottschalk et al indicated that the main role of the GMed would be to compress the head of the femur into the acetabulum (hip socket) during locomotion and to help in stabilizing the pelvis on the femur in single leg stance. Then They put forward the idea that each of the three different heads of the muscle performs a unique role in locomotion:
The posterior fibres contract in first posture phase to lock the ball into the socket. This idea is supported by the observation the anterior fibers possess an almost parallel alignment with the neck of the femur. The posterior fibres therefore perform a compressing or stabilizing function for the hip joint.
The middle/anterior fibers, that run into a direction, help to begin. These fibers operate synergistically with TFL in stabilizing the anus on the femur, to protect against the other side falling (or Trendelenburg). The investigators point out that the TFL has the role in stabilizing the pelvis on the cool; this action, analogous to the way the supraspinatus from the shoulder helps the potent deltoid in shoulder abduction is only assisted by the GMed. The anterior fibres enable the femur to rotate to the hip joint. This is essential for rotation, so the side leg can swing forward during gait. The anterior fibers play this role. So Gottschalk et al hypothesized the primary functions of the GMed are:
1. To stabilize the femur on the ilium (pelvic stability)
2.) To behave as hip rotators
3. To approximate the head of the femur in effect producing a hip joint that is very tight and secure .
Investigators have found on cadaver studies that GMed has a large physiological cross-sectional region and short fibre lengths and therefore is able to generate large forces over a narrow range of spans(16). They postulate the GMed really functions in hip/pelvic that is impartial postures as it would when stabilizing cool and the pelvis during single leg stance. Exercises which induce the GMed into excessively shortened or lengthened positions may in fact not target the GMed but additional hip abductors/external rotators. Therefore it should be the dominant of the hip abductors, GMed gets the CSA of the hip abductors. As it has fibres which are packed together it can produce a whole lot of force. But is does not create large forces. It is designed to work and stabilize the fashionable.
Injuries To The Gluteus Medius
Dysfunction from the GMed has been associated with a variety of musculoskeletal pain syndromes. It’s thought that these injuries are a result of the inability of the GMed to control alignment and movement in the pelvis, femur and tibia. These harms include but are not Limited to:1. Patellofemoral pain syndromes(15)
2. Lumbar spine issues(11)
3. ITB friction syndromes(8)
4. Hip joint pathology(10).
It’s Been assumed for some time that hip internal rotation is an unwanted pathomechanic of the hip joint as hip rotation will allow the femur to migrate inwards and make valgus collapse at the knee. The premise has been extrapolated to suggest that this hip internal rotation is a result of other fashionable joint rotators along with weak GMed. However, the job from Ward et al (2011)(16) suggest that in reality the GMed seems to function better physiologically if the hip is placed in some internal rotation. Is this internal rotation a compensation to permit the GMed to be recruited at the presence of weakness of additional hip muscles like other deep hip rotators and the gluteus maximus?
Injuries to the GMed such as tendon tears, pressure injuries, trigger factors and related bursitis also have been credited to having weak GMeds (3,12,13).
Rehabilitation Exercises Gluteus Medius
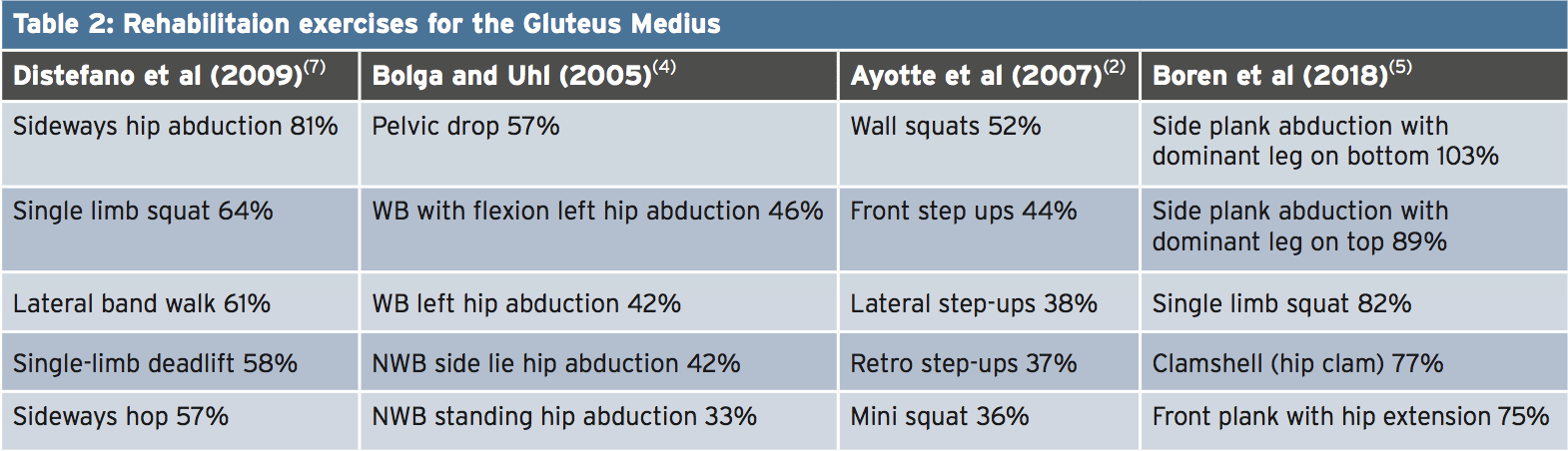
A wide selection of studies have examined the purpose of this GMed whilst doing a variety of lower limb exercises(1,2,4,5,6,7). These studies base their decisions on comparative electromyographic (EMG) data during certain exercises. The top five exercises in each study are presented in Table 2 and viewers can be made on the exact exercises. The percent exhibited along with the exercise is the \% of Maximal Voluntary Contraction (MVC) of those GMed. It needs to be pointed out that differences in activity between writers may differ due to a number of Factors like:1. EMG positioning
2. Electrical interference from different muscles
3. Differences in the precise mechanics of the exercises that are chosen.
The EMG data does not necessarily inform us if the action is being created by the GMed or just stabilizing the hip joint and anus similar to the rotator cuff muscles work during shoulder abduction and flexion movements, whilst muscles are functioning.
In a recent study, researchers looked at the relative contribution between the GMedand that the TFL and recognized these five exercises that best used GMed with nominal TFL(14):
1. Clam with theraband
2. Sidestep with theraband
3. Unilateral bridge
4. Quadruped hip extension, knee stretching
5. Hip extension.
With so many variations in the potential beneficial exercises which might be utilized to strengthen the GMed, often exercise utilized by the therapist’s choice may be a ‘horses for courses’ approach. Posture variations might be used if the person feels pain on weight bearing movements then. The customer may not ‘sense’ the motion needed therefore exercises. Often it may be the therapist’s personal choice regarding what they perceive to be the best GMed exercise. Furthermore, it could be argued that what a customer feels in and around their hip may be GMed hip abductors like gluteus minimus and/or other hip rotators like muscles that were gemellus, the obturator group femoris and piriformis. Studies are needed utilizing both fine wire EMG and surface EMG on muscles to elucidate the connections between these muscles’ contribution.
The 3 exercises are variations on exercises. The reason they have been contained is to meet the work by Gottschalk et al(9) which demonstrates that GMed operates in varying ways throughout hip flexion to extension as demonstrated from the gait cycle, as well as the work by Ward et al(10) which suggests the muscle operates through quite unbiased hip/pelvic positions and works essentially isometrically or through quite short ranges of movement. What’s more, the 3 exercises mimic weight bearing through the hip joint, making them functional concerning activation in weight bearing positions or attempt to either weight bear.
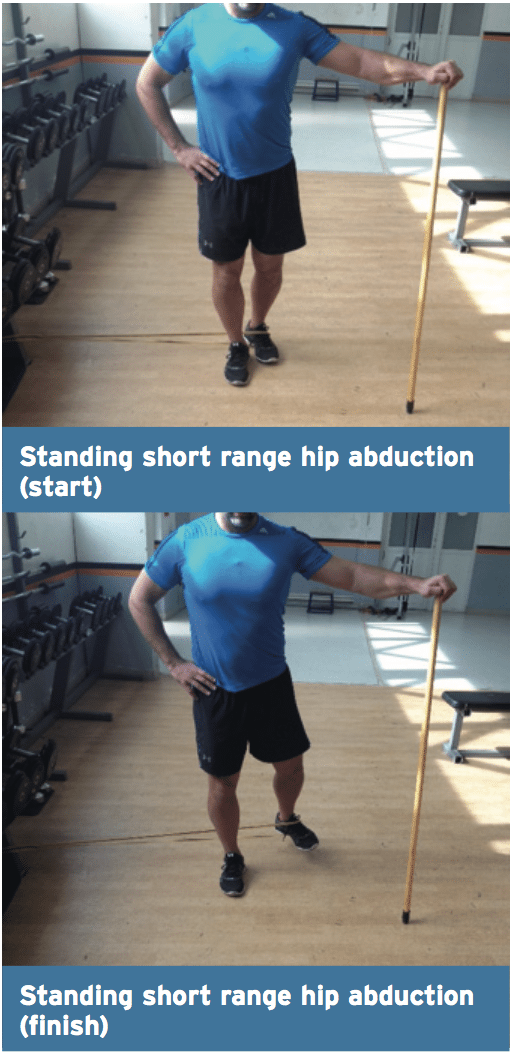
1. Standing Short Range Hip Abduction
A. Stand with a band around the foot and the hand on exactly the exact same side reinforced by a broomstick for equilibrium.
B. Gently move the banded leg to abduction/external rotation/extension.
C. The stance limb is in slight hip flexion and stays in this position.
D. Perform 8-10 repetitions of slow hip abduction/external rotation/extension.
E. This will be felt at both the stance side GMed (in little hip flexion) as well as the abducting side GMed (right into small hip expansion).
2. Kneeling Clam
A. Kneel on a seat with a band wrapped round the knees. Feet are kept together.
B. Hold onto a broomstick for equilibrium.
C. Gently move down the knees whilst keeping up the foot contact. This moves the fashionable to slight rotation.
D. Perform sets of 10-15 repetitions and ensure the movement is kept small (2-3 inches .
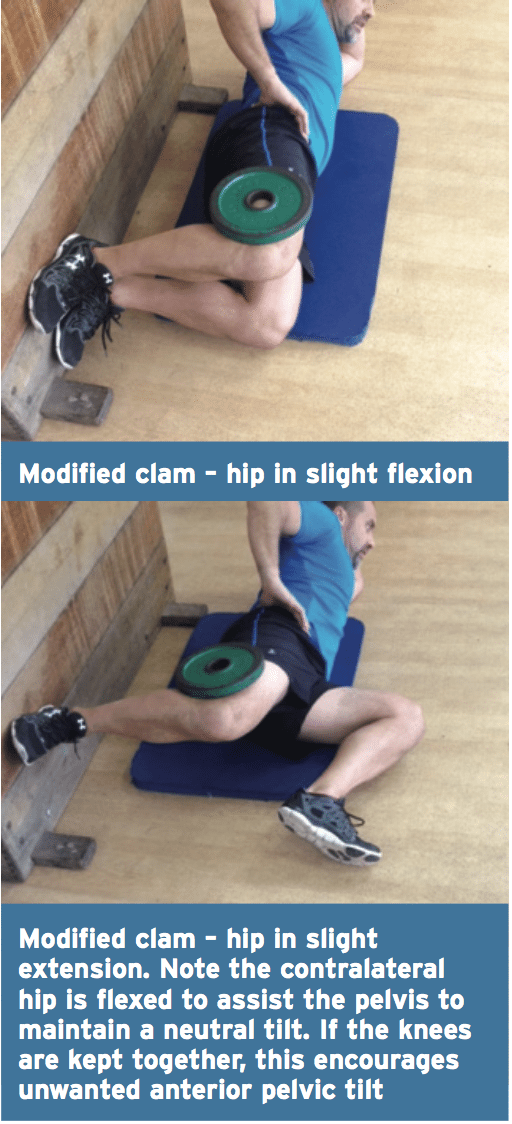
3. Modified Clam
Conclusion
The GMed is a muscle which has received a lot of attention and research in the past couple of decades. Research to the GMed using cadaveric studies , biomechanical modeling and EMG have concluded that it is an important muscle that needs to be strengthened to assist in control, hip joint stability and reduced limb kinetic control. This article presents the applicable and up-to-date anatomy and biomechanical awareness the research on the author’s suggestions on some exercises as well as activation in workout that may work the GMed muscle, on the muscle building.References
1. Arch Phys Med Rehabil; 1999. 80:842-850.
2. J Orthop Sports Phys Ther; 2007. 37: 48-55.
3. The Iowa Orthopedic journal. 2003. 23; pp57-60.
4.J Orthop Sports Phyl Ther; 2005. 35: 488-494.
5. International Journal of Sports Physical Therapy. 2011. 6(3). 206-223.
6. J Sport Rehabil; 2009. 18:91-103.
7. J Orthop Sports Phys Ther; 2009. 39: 532-540.
8. J Orthop Sports Phys Ther; 2010. 40:52-58.
9. Journal of Anatomy. 1989. 166: 179-189.
10. Man Ther. 2009;14:611-617.
11. Arch Phys Med Rehabil; 1998. 79:412-417.
12. AJR. 173(4); 1123-1126.
13. Eur Radiol. 2006. 17(7); pp 1172-83.
14. Journal of Orthopaedic and Sports Physical Therapy. 2013. 43(2); 54-65.
15. J Orthop Sports Phys Ther. 2009. 39:12-19.
16. Journal of Orthopaedic and Sports Physical Therapy. 2011. 40(2); 95-102.