A majority of complications to the hip joint can often be related to acetabular labral tears, or ALT, and in up to 80 percent of cases, these can also be
identified alongside intra-articular snapping hip syndrome. Labral tears in the
joints of the hip account for hip and groin pain symptoms of approximately
22-55 percent of individuals affected by the injury. Research suggests that an
untreated ALT may increase the risk of degenerative hip arthritis, which has
created a widespread interest within many healthcare professionals.
In the past ten years, the examination and imaging techniques utilized
to diagnose acetabular labral tears have been increasing greatly, although
these assessments are still considered to be complex. Foremost, by reviewing
the anatomy and biomechanics of the acetabular labrum, the evaluation
techniques and the treatments, individuals can learn to understand the options
for managing their labral tears.
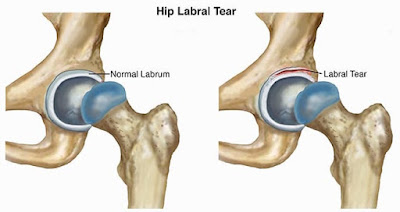
Anatomy of the Hip
The labrum increases the surface area of the acetabulum by 22 percent
while it increases the volume by 33 percent, functioning accordingly to fasten
the head of the femur while allowing it to rotate. From a cross-sectional view,
the labrum is triangular in shape with an extra articular area of thick
connective tissue which contains a rich supply of blood while the intra
articular area majorly has no blood supply.
When the hip’s normal range of mobility extends beyond its limit, the
labrum is stressed by a strong, compressive force and a tear at his point can
ultimately affect the stability of the joint and distribution of weight or
load. Furthermore, the labrum is considered a pain generating structure as numerous
pain receptors are located in its superior and anterior regions. It is at the
anterior surface where an ALT is most vulnerable to pressure along the end
point of hip flexion. On another note, abnormal alterations within the
structure, such as retroverted acetabulum and coxa valga, have been simultaneously
recorded in up to 87 percent of individuals with labral tears.
Evaluating Acetabular Labral Tears
Acetabular labral tears are difficult to diagnose and, despite of current
advances in medical imaging and assessment techniques, one report established
that on average, patients with an ALT visited three healthcare providers and
waited for approximately 21 months before the injury was properly diagnosed. As
a medical professional evaluates an individual with a suspected hip injury, femoro-acetabular
impingement, or FAI, and acetabular cartilage damage as well as MRI imaging
should be utilized to further support a diagnosis.
Acetabular labral tears are often caused by cutting, pivoting, twisting
and repetitive movements from end range hip flexions frequently practiced among
tennis players, football players and runners. Researchers from the New England
Baptist hospital in Boston, USA identified 273 athletes who also had articular
cartilage damage from the 436 labral tear arthroscopies analyzed, almost 62
percent. However, the exact nature of an ALT injury may not always be clear to
the individual, as these may also be degenerative, congenital or traumatic in
its occurrence.
During a physical assessment for any hip-related injuries, it is
essential to be observant of other non-musculoskeletal related pathologies. Hip
pain may be associated to acetabular labral tears but hip complications can
also be the result of lumbar spine or pelvic girdle dysfunction, abdominal
viscera and issues with the peripheral nervous system. Symptoms of pain while
resting, pain at night, fever, night sweats, unexplained weight loss are
indicators of a non-musculoskeletal pathology which may require referral for
further examination by a specialized healthcare provider. Hip pain may also be
related to the abdominal and pelvic organs and a musculoskeletal injury must
not be presumed.
An individual with an undiagnosed ALT may also be affected with
synovitis and experience joint inflammation which can force them to adopt
positions of hip flexion, external rotation and slight abduction, causing the
capsule to be at its largest potential volume to reduce the stress on the
labrum. Positions which include flexion and or abduction have been determined
to increase the overall weight on the labrum and these are consciously avoided.
The joined, compressing position of flexion, abduction and internal rotation,
best referred to as FADDIR’s test, increases stress to the labrum but it is
also a contributor to intra-articular hip pathology. Individuals with
acetabular labral tears may also report pain while squatting, stepping up with
the affected extremity, or while sitting in a chair with the hips positioned
lower than the knees. Additionally, an individual with an ALT is unlikely to
extend the hip fully when running as this places the greatest amount of weight
to the anterior joint capsule, subsequently adding stress to the anterior
labrum.
Surgical versus non-surgical treatment
Hip
arthroscopy is a popular treatment utilized for individuals presenting symptoms
of an ALT longer than four weeks, which has also been confirmed by MRI, or
magnetic resonance imaging, and/or MRA, or magnetic resonance arthrogram. Hip arthroscopy
for an ALT may include either labral debridement or labral repair. Different
from surgical repair, there is limited support for conservative treatments for acetabular
labral tears. However, researchers from Sao Paulo, Brazil have provided a case
series of four individuals that underwent a rehabilitation program for this
type of hip injury without surgery. The four individuals were diagnosed by an
MRI scan and underwent a 3-phase program with the first being pain control, hip
stabilization, re-education and correction of abnormal joint movement. Phase
two focused on restoring normal range of motion, muscular strength and started
sensory motor training. The final phase of their rehabilitation program focused
on preparing the athlete to return to their specific sport.
The four individuals involved in the case series were in their mid-twenties
and were from both sedentary and athletic backgrounds. The outcome of the
conservative rehabilitation program leads to the individual’s pain level
decrease, improved function and corrected muscle imbalances. Their muscle strength
increased with the hip flexors from 1 percent to 39 percent, hip abductors
increased muscle strength from 18 percent to 56 percent and the hip extensors
increased their muscle strength from 68 percent to 139 percent. The results of
the research were considered limited, as the case series only evaluated four
individuals but nevertheless, the outcome could provide a proper approach while
a patient is awaiting an arthroscopy.
Rehabilitation
After undergoing surgery for an ALT, the evidence behind following
through with rehabilitation is considered limited as well in terms of its
evidence, both within the surgeons own rehabilitation protocols and the
therapist’s expertise. Researchers from Tampa, USA, constructed a
rehabilitation protocol for the patients to follow which the following protocol
is largely based upon:
Phase 1 (weeks 1–4)
After experiencing an ALT, or acetabular labral tears, the individual
should limit the amount of weight they place on their limb by 50 percent for
approximately 7-10 days, with flexion limited to 90° for 14 days. A labral
debridement, or the removal of damaged tissue or foreign objects from a wound, has
no limits following a surgical procedure into abduction, internal or external
rotation or extension. In contrast, repairing acetabular labral tears should
maintain non-weight bearing or toe-touch weight bearing for three to six weeks after
a surgical operation.
During labral repair, the individual should maintain conservative ranges
of movement while internal and external rotation should be conservatively moved
into for 3 weeks. It’s essential to remember that if other procedures are
carried out, such as micro fracture repair, then protocols following a surgery
may be different.
In the immediate time period following a surgical operation, it is
essential to manage pain, reduce swelling and begin early carefully moving the
affected limb, but it is also essential to focus on other factors such as core activation
and abductor control. Decreased activity of the hip abductor muscles has been previously
linked to various lower extremity injuries and symptoms, including anterior
knee pain. Therefore, once the individual begins to restore the natural range
of their hip, it is essential to encourage them to activate the deep hip and
trunk stability muscles to prevent secondary injuries from developing in the
future.
Phase 2 (weeks 5–7)
During this stage of rehabilitation, it is essential to restore normal
range of movement while focusing on increasing strength and developing
flexibility of the muscles crossing the hip joint.
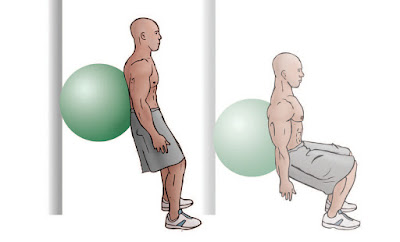
Double Leg Standing Squats w/ Swiss Ball
Seated Resistance: Internal/External Rotation
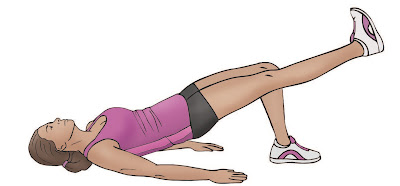
Double - Single Leg Bridging
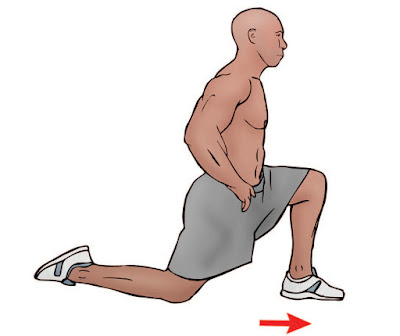
Kneeling Hip Flexor Stretches
Side Stepping w/ Band Around Knees
Phase 3 (weeks 8-12)
While in this phase, the individual has a great opportunity to develop
cardiovascular fitness and functional control of their hip. Functional
stability exercises should be practiced in a standing position, making sure to maintain
and improve stability in order for the individual to be able to return to their
normal sport participation. Exercises to include in this phase are walking
lunges, lunges with trunk rotation over the front leg and a Swiss ball program
appropriate for challenging the core muscles.
Phase 4 (weeks 12+)
This phase of the rehabilitation program includes preparing the athlete
for their return to their specific sport, emphasizing on specific protocols to
train the individual around the task they will be performing. If the athlete is
a defender in football, they should be replicating tasks specific to their
position. Prior to the individual resuming full training, they must be able to
demonstrate the same neuromuscular control as the unaffected side.
In conclusion, an individual with suspected acetabular labral tears should have their
injury confirmed using an MRI or MRA to properly determine the presence of an
ALT but also to exclude any referred pain which could be signaling the presence
of another musculoskeletal injury. An appropriate rehabilitation program should
be started immediately to improve the function of the hip, control and to
manage pain and ultimately restore the individual’s overall health. This will
allow the athlete to proceed through any procedures with greater ease having
already commenced a rehabilitation program.
Chiropractic and Athletic Performance
By Dr. Alex Jimenez