The piriformis muscle is commonly known among athletes and healthcare
professionals as a significant muscle in the posterior hip. This muscle
functions to control hip joint rotation and abduction and it is also a distinguishable
muscle due to its inversion of action in rotation. The piriformis muscle also raises
awareness as the various causes of piriformis muscle syndrome, a condition suspected
to be a potential source of pain and dysfunction, not only in athletes, but in
the general population as well.
Anatomy of the Piriformis Muscle
The piriformis muscle originates on the anterior surface of the sacrum
and it is securely held to it by three tissue attachments found between the
first, second, third and fourth anterior sacral foramina. Occasionally, its
origin may be so broad that it joins the capsule of the sacroiliac joint with
the sacrotuberous and/or sacrospinous ligament. The piriformis muscle is a thick
and strong muscle that travels out of the pelvis through the greater sciatic
foramen, dividing the foramen into the suprapiriform and infra-piriform
foramina. As it courses through the greater sciatic foramen, the muscle
decreases to a point where it forms a tendon that attaches to the
superior-medial surface of the greater trochanter, frequently integrating with
the tendon of the obturator internus and gemelli muscles.
 |
| Share Free Ebook |
The piriformis muscle is closely associated with other short hip
rotators as well, such as the superior gemellus, obturator internus, inferior
gemellus and obturator externus. The primary difference between this muscle and
other short rotators is its connection to the sciatic nerve. The piriformis
muscle passes behind the nerve while the other rotators pass before it.
Anatomical Variants
Several anatomical variations have been previously diagnosed among the
piriformis muscle. First, there may be additional medial attachments to the
first and fifth sacral vertebrae and to the coccyx. Second, the tendon may
merge with the gluteus medius or minimus or with the gemellus. Also, in
approximately less than 20 percent of cases, the piriformis muscle may be
divided into two different segments, through which part or all of the sciatic
nerve may travel. Then, the muscle may blend with the posterior hip joint
capsule as a conjoined tendon with the obturator internus. Additionally, the
distal attachment of the piriformis muscle has been demonstrated to vary in
proportion and position on the supero-medial surface of the greater trochanter.
It can stretch across 25 to 64 percent of the anterior-posterior length along
the greater trochanter, with 57 percent of it attaching more anteriorly and 43
percent more posteriorly. Last but not least, researchers studied its insertion
point broadly and discovered that four types of insertions existed and these
were characterized based on the relationship to the obturator internus. The
variation of placement and width of the distal attachment of the piriformis
muscle may influence the effectiveness of the concept known as the inversion of
action.
Furthermore, the connection between the piriformis muscle and the
sciatic nerve has been a highly debated complication. It’s been previously
concluded that there are several anatomical variations among the piriformis
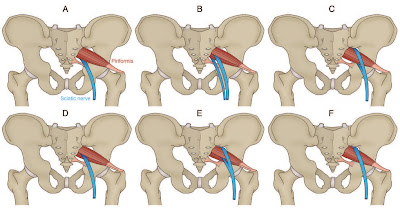
muscle and its connection to the sciatic nerve. The sub-types of this variation
include: type 1-A, where the muscle is pear shaped with the nerve running
anteriorly and inferiorly to this, found in 70 to 85 percent of cases; type 2-B,
where the piriformis muscle is divided into two sections with the common
peroneal nerve running between the two parts and the tibial nerve travels
anteriorly and below, found in 10 to 20 percent of cases; type 3-C, where the
peroneal portion loops over the top of the muscle and the tibial portion is
found below, found in 2 to 3 percent of cases; and type 4-D, where the
undivided nerve passes through the piriformis muscle, found in approximately 2
percent of cases.
Moreover, it is also speculated that two other, very rare variations may
occur, demonstrated by letters E and F in the diagram. Type 1-A is the most
common variation, displaying the sciatic nerve as it passes below the
piriformis muscle.
Function of the Piriformis Muscle
The
fundamental functions of the piriformis muscle are to provide hip external
rotation and allow abduction at 90 degrees of hip flexion. During
weight-bearing, the piriformis muscle restricts femoral internal rotation in
the stance phase of walking and running. Also, it assists the short hip
rotators in compressing the hip joint and stabilizing it. Because it can exert
an oblique force on the sacrum, it may produce a strong rotary shearing force
on the sacroiliac joint. Otherwise, this would dislocate the ipsilateral base
of the sacrum forward and the apex of the sacrum backwards.
Since the piriformis muscle is the furthest behind of the hip external
rotators because of its attachment on the anterior surface of the sacrum, it
has the greatest influence to apply a rotation effect on the hip joint. Occasionally,
healthcare specialists have found issues with the piriformis muscle where it appears
to be tight and hypertonic, while the other short hip rotators which are found closer
to the axis of rotation become inhibited and hypotonic.
Inversion of action
The most argumentative complication relating to the function of the
piriformis muscle is its reversal-of-function role, best referred to as the inversion
of action role. Researchers have suggested that as the hip approaches angles of
60 to 90 degrees and greater, the tendon of the piriformis muscle shifts on the
greater trochanter. As a result, its line of pull becomes ineffective as a hip
external rotator, however, it does contribute to internal hip rotation.
Consequently, it reverses its rotation function at high hip flexion angles.
The role of the piriformis muscle at several joint angles is an
essential consideration for healthcare professionals who evaluate and treat the
causes of piriformis syndrome. Frequently, it’s recommended to stretch the hip
into flexion, adduction and external rotation to stretch the piriformis muscle
over the glutes by utilizing the reversal of function concept.
Nonetheless, more recent studies conducted through anatomical dissection
have demonstrated that the attachment of the piriformis muscle onto the greater
trochanter can change and, in some instances, it may insert in a position by
which it may be unable to reverse its function, for example, in a more
posteriorly placed attachment. Thus, stretching the piriformis muscle into
external rotation when the hip is flexed beyond 90 degrees, based on the
inversion of action role, would be ineffective as a treatment or misleading as
an examination technique.
MSK Dysfunction and Causes of Piriformis Syndrome
Many decades
ago, it was suggested that in some cases, sciatica symptoms may originate
outside the spine as a result of the piriformis muscles. This hypothesis was
supported soon after when specialists successfully improved an individual’s
symptoms of sciatica by surgically dividing the piriformis muscle. Based on
cadaver anatomical dissections, the researchers believed that the spasm of the
piriformis muscle could be responsible for the irritation of the sciatic nerve.
The medical term piriformis syndrome then became associated to sciatica
symptoms, believed to be caused by a usually traumatic abnormality in the
piriformis muscle with a focus on ruling out more common causes of sciatica,
such as nerve root impingement caused by a disc herniation. It soon became an
accepted interpretation but with no consensus about the exact clinical signs
and diagnostic tests to differentiate it from other sources of sciatica.
Understanding the Causes of Piriformis Syndrome
Piriformis syndrome can be defined as a clinical entity whereby the
interaction between the piriformis muscle and the sciatic nerve may irritate
the nerves and develop posterior hip pain with distal referral down the
posterior thigh, resembling symptoms of true sciatica. Distinguishing the
damage to this region typically follows exceptions of the more common causes of
sciatica and buttock pain.
More specifically, reports of buttock pain with distal referral of symptoms
are not unique to the causes of piriformis syndrome. Similar symptoms are prevalent
with the more medically evident lower back pain syndromes and pelvic
dysfunctions. Therefore, a complete evaluation of these areas must be performed
to rule out any underlying pathology. It has been suggested that the causes of piriformis
syndrome can be held responsible for approximately 5 to 6 percent of sciatica
cases. In the majority of instances, it develops in middle-aged individuals, an
average or 38 years and it’s more common among women.
Pathogenesis of Piriformis Syndrome
The causes
of Piriformis syndrome can be associated to three primary causing factors:
First, the referred pain may be the result of myofascial trigger points.
Second, the entrapment of the nerve against the greater sciatic foramen as it
passes through the infrapiriform fossa or within a variating piriformis muscle.
And third, sacroiliac joint dysfunction causing piriformis muscle spasms.
Other
researchers presented an additional number of factors behind the causes of
piriformis syndrome as follows: gluteal trauma in the sacroiliac or gluteal
regions, anatomical variations, myofascial trigger points, hypertrophy of the
piriformis muscle or spasms of the piriformis muscle, secondary to spinal
surgery such as laminectomy, space occupying lesions such as neoplasm,
bursitis, abscess and myositis, intragluteal injections and femoral nailing.
Symptoms
The general symptoms described with the causes of piriformis syndrome
include: a tight or cramping sensation in the buttock and/or hamstring, gluteal
pain in up to 98 percent of cases, calf
pain in up to 59 percent of cases, aggravation through sitting and squatting if
the trunk is inclined forward or the leg is crossed over the unaffected leg and
possible peripheral nerve signs such as pain and paresthesia in the back,
groin, buttocks, perineum and back of the thigh in up to 82 percent of cases.
Physical findings and examinations
When palpable
spasm within the surrounding piriformis muscle occur and there is obturator
internus pain and external tenderness over the greater sciatic notch, found in
approximately 59 to 92 percent of cases, the individual must perform the Sims
position to follow up an evaluation. The piriformis line should overlie the
superior border of the piriformis muscle and extend immediately from above the
greater trochanter to the cephalic border of the greater sciatic foramen at the
sacrum. The examination will continue where the line is divided into equal
thirds. The fully rendered thumb presses on the point of maximum trigger-point
tenderness, which is usually found just lateral to the junction of the middle
and last thirds of the line.
It’s important to keep in mind that hip
flexion with active external rotation or passive internal rotation may aggravate
the symptoms of dysfunction. Additional findings for the evaluated causes of
piriformis syndrome have demonstrated a positive SLR that is less than 15
degrees on the normal side. Other tests used to evaluate the causes of piriformis
syndrome include, positive Freiberg’s sign, used in 32 to 63 percent of cases,
involves the reproduction of pain on a passively forced internal rotation of
the hip in the supine position, believed to result from passive stretching of
the piriformis muscle and pressure of the sciatic nerve at the sacrospinous
ligament. Pacers sign, used in 30 to 74 percent of cases, involves reproducing
pain and weakness on resisted abduction and external rotation of the thigh in a
sitting position. Pain in a FAIR position used to evaluate dysfunction,
involves the reproduction of pain when the leg is held in flexion, adduction
and internal rotation. Furthermore, an accentuated lumbar lordosis and hip
flexor tightness predisposes an individual to increased compression of the
sciatic nerve against the sciatic notch by a shortened piriformis.
Electro-diagnostic tests may also prove useful to diagnose piriformis muscle
complications.
Investigations
Conventional imaging, such as X-ray, CT scan and MRI, tend to be
ineffective in diagnosing the presence and causes of piriformis syndrome. However,
some value may exist in electro-diagnostic testing. The purpose of these tests
is to find conduction faults in the sciatic nerve. Findings such as
long-latency potentials, for instance the H reflex of the tibial nerve and/or
peroneal nerve, may be normal at rest but become delayed in positions where the
hip external rotators are tightened.
It’s been established that the tibial division of the sciatic nerve is
typically spared, the inferior gluteal nerve that supplies the gluteus maximus
may be affected and the muscle becomes atrophied. However, testing of the
peroneal nerve may provide more conclusive results as they’re more likely to be
the impinged portion of the sciatic nerve. The H-wave may become inactive
during the painful position of forced adduction-internal rotation of the
affected leg.
Piriformis Syndrome Myths
Researchers
argued that piriformis syndrome is a frequently over-used term to describe any
non-specific gluteal tenderness with radiating leg pain. It was discussed that
only in rare cases is the piriformis muscle involved in nerve compression of
the sciatic nerve to legitimately qualify as one of the causes of piriformis
syndrome. It was cited that there is only limited evidence and cases where the
diagnosis of the causes of piriformis syndrome can be made. First, where there
is compressive damage to the sciatic nerve by the piriformis muscle. In several
isolated studies, the sciatic nerve was seen to be compressed by the piriformis
muscle in instances such as hypertrophy of the muscle, general anatomical abnormalities
such as a bifid piriformis muscle and due to compression by fibrous bands.
Also, trauma and scarring to the piriformis muscle can involve the
sciatic nerve. It is possible that rare cases of true piriformis syndrome have
been caused by direct heavy trauma to the piriformis muscle due to a blunt
trauma to the muscle. This is termed as post- traumatic piriformis syndrome.
Researchers supported this argument by stating that it is more likely
that, given the anatomical relationship of the piriformis muscle to the various
nerves in the deep gluteal region, the buttock pain represents entrapment of
the gluteal nerves and the hamstring pain entrapment of the posterior cutaneous
nerve of the thigh, rather than the sciatic nerve alone. This demonstrates the
medically analyzed circumstance in the absence of distal sciatic neurological
signs. Whether the piriformis muscle is the cause of the compression has not
been clearly established. It is possible that the obturator internus/gemelli
complex is an alternative cause of neural compression. The researchers have
suggested utilizing the term deep gluteal syndrome rather than piriformis
syndrome.
Treatment
When it is believed that a factor which is considered one of the several
causes of piriformis syndrome exists and a healthcare professional feels that a
proper diagnosis has been made, the treatment will usually depend on the cause
behind the dysfunction. If the piriformis muscle is tight and it spasms, then
initially conservative treatment will focus on stretching and massaging the
tight muscle to remove the piriformis muscle as being the source of the pain.
If this fails, then the following have been suggested and may be attempted:
local anesthetic block, typically performed by an anesthesiologist who has
expertise in pain management and in performing nerve blocks; steroid injections
into the piriformis muscle; botulinum toxin injections in the piriformis
muscle; and surgical neurolysis.
Therapist-directed interventions, such as stretching of the piriformis
muscle and direct trigger point massage, can also be used as treatment. It’s
been encouraged that piriformis muscle stretches are done in positions of hip
flexion greater than 90 degrees, adduction and external rotation to utilize the
inversion of action effect of the piriformis muscle to isolate the stretch to
this muscle independent of the other hip external rotators.
However, recent evidence utilizing ultrasound investigation demonstrated
that there was no interaction between hip flexion angle and the thickness of
the piriformis muscle tendon in both internal and lateral hip rotation
stretching, which suggests that the piriformis muscle does not invert its
action. Furthermore, researchers who performed cadaveric studies found that the
piriformis muscle insertion is a lot more complex and varied than initially
believed. It is possible that the piriformis muscle may invert its action only
in some subjects but not in others.
As a result, due to the disagreements and confusions over the inversion
of action concept, it is recommended that healthcare professionals should
performs two variations of a piriformis muscle stretch: stretches in flexion,
adduction and external rotation and stretches in flexion, adduction and
internal rotation.
Pigeon Stretch for left PM: hip flexion, neutral adduction and maximal hip rotation.
Stretch for left PM: hip is in flexion, neutral adduction and maximal external rotation.
Short leg posterior chain stretch for right PM: hip is in 90 degree flexion, adduction and neutral rotation.
Trigger Points and Massage
The most appropriate suggestion to palpate the piriformis muscle trigger
points is in the following recommended position. In this posture, the
healthcare professional can feel for the deep piriformis muscle trigger points
and apply a constant pressure to relieve the trigger points as well as apply a
flush massage to the muscle in this position. In this position, the large gluteus
maximus is relaxed and it is easier to feel the deeper piriformis muscle.
The piriformis muscle is a deep posterior hip muscle that is closely
related anatomically to both the sacroiliac joint and the sciatic nerve. It is
a muscle that is a dominant hip rotator and stabilizer, with a tendency to
shorten and become hypertonic. Therefore, stretching and massage techniques are
best recommended and utilized to reduce the tone through the muscle. In
conclusion, it has also been suggested in compression and irritation of the
sciatic nerve, most commonly referred to as piriformis syndrome.
By Dr. Alex Jimenez