Chiropractic injury specialist, Dr. Alexander Jimenez examines a preventive injury approach based on the very best of what's known.
In sports medicine, there's not any tougher challenge than hamstrings -- often our most commonly seen injury, as well as uncomfortably significant re-injury rates. With a growing amount of research in this area(6), this is a good time to bring the literature together and invent an evidence-based method of preventing hamstring injury and recurrence.
Injury incidence
It is painfully easy to find evidence. Various sports report high squad incidences of hamstring injury, for example:- 18% and 20% per season among sprinters.
- 40% over two seasons among track and field athletes.
- 12%,16%, and 23% per season in Australian Rules footballers(8,2,9,10,11,12).
- In one sprint season, every second injury was to a hamstring(8).
- 12% and 13-16% of injuries per season in soccer(2, 3).
Risk Factors
The logic of identifying risk factors is to modify these so as to decrease injury levels. We will need to know not just which factors are risky, but just how they influence harm.Modifiable Factor 1): The Hamstrings
Powerful recent evidence implicates strength shortages as a pre-disposing factor for hamstring injury. The imbalances usually analyzed are: hamstring to quad (H:Q); eccentric to concentric (E:C); and side to side (S:S). By comparison, the demand for hamstring flexibility is much less apparent in the signs.Since 2008 a number of isokinetic strength studies, such as a very large one, have shown isokinetic strength shortages to be predictive of hamstring injury. Back in Hong Kong, athletes using a diminished H:Q had 17 times increased risk of hamstring injury (8) and in elite Japanese sprinters S:S weakness has been correlated with hamstring injury(two).
One of 462 Belgian soccer players, the injury rate was considerably higher among gamers with isokinetic power imbalances, compared to those without(6).
Past injury is an integral factor (see below), and a study may help us to understand why. It reports that optimum length (ie, the best muscle length for active stress) has been found to be briefer in formerly injured muscles. Reduced/shorter 'optimal span' could perhaps predispose the hamstring to injury during eccentric loading in its outer variety (ie, once the muscle is nearing full stretch)(16).
The role of hamstring flexibility remains unclear: one study (Aussie Rules) revealed that sit-and-reach evaluation results didn't correlate with cerebral muscle injury(11). In a bigger Belgian soccer study, nevertheless, those injured had previously had considerably bad hamstring flexibility(17).
Modifiable Factor 2): Other Structures
One of Aussie rules players, too little flexibility in quadriceps(18) and hip flexors(19) has been predictive of hamstring injury. The same studies investigated restricted ankle dorsiflexion and concluded that this could have some relevance(19). I discuss this below.Weak gluteals are implicated due to their job as concentric hip extensors. It has been proven that sprinters with S:S fatigue in concentric hip expansion were more prone to hamstring injury on the weak side(two). Equally all pelvic muscles help to maintain pelvic stability and hence reduce injury threat(41).
Non-Modifiable Risk Factors
Although the following factors are unalterable, it makes great sense to consider these when targeting particular players for preventive programs, especially in the event that you don't have access to expensive and time consuming isokinetic testing.Two studies found the best risk factor for a previous posterior thigh injury (12) or a past history of hamstring injury (19). This goes some way to describing recurrence rates touching 40% in 1 study(3).
Some studies confirm that age is a factor, with older players at elevated risk(12,19,18,1). Players of black cultural origin(1) and Aboriginal descent(12) have been demonstrated to be more than averagely vulnerable.
If, for instance, you're responsible for a black 29-year-old participant with a hamstring injury background, you'll have both rationale and evidence to direct your use of a preventive program with that individual.
Mechanism Of Injury
To examine more precisely the mechanism of harm, we must consider the part of the hamstring muscle. Injury generally occurs in a sprinting scenario. Quick active extension of the knee requires the hamstrings to act eccentrically to decelerate the late swing-phase; but then they have instantly to change to concentric loading during early stance phase, where they behave as hip extensors(20). This stage sets the hamstrings in their outer range, in the very moment they have to make the greatest effort. Fig 1 (below) helps illustrate how these risk factors interact.Most injuries include the biceps femoris muscle(1,47). This might be because at sprints of 80 percent to 100% of high speed, summit lengths are significantly longer and occur later than in another hamstring muscles(23). In this last period of gait, a high-force stretch-shortening cycle happens, and the hamstring unit relies on its non-contractile component to absorb, then generate force(22,24).
We can now start to learn the way the reduced isokinetic strength profile could cause hamstring overload and injury.
Hamstring flexibility becomes an issue if you regard that harm happens in late swing/early posture stage, once the muscle is lengthened. Logically, a short muscle must invest additional time in its outer range (ie, slightly lengthened under pressure) so as to come up with a typical powerful stride length. This places the lengthened hamstring under more stress and might explain why short hamstrings can be prone to trauma(17). In the exact same way that 'optimum length' (the muscle's optimal length for active tension) is found to be shorter in previously injured muscles (see above), this decreased length could also predispose the hamstring to injury in the exact situation(16).
The Fatigue Factor
And here is something you may discover surprising: there's a strong rationale and a few evidential back-up to imply that both general aerobic and particular hamstring endurance operate are strongly implicated in injury.Hamstring injuries are most frequent during rivalry(1), even when effort should be at its highest. It is well known that in football a significant increase in injury is observed toward the end of each half(1). This may well be explained by the reduction in bizarre hamstring torque generation and operational power ratio -- caused by fatigue -- which players tend to suffer from at the conclusion of football halves. The angle of peak torque generation increases significantly (ie, the best length gets shorter) as every half goes on(42). Other factors include:
- Muscle elasticity (which buffers the muscle fibers) reduces with length(48)
- Fatigued muscles consume less energy before they fail(26)
- Hamstrings fatigue comparatively faster than their antagonist, which will affect the H:Q ratio adversely(27).
It's A Multi-Factorial Thing
Fatigue is not likely to be the sole factor in play. Here are some other prime contributors to injury:Hip flexor length is as important as hamstring length(48). The two rectus femoris and hip flexors can anteriorly rotate the pelvis. In late-stance stage, brief contralateral (opposite side) hip flexors will rotate the anus relatively anteriorly; and in late-swing phase the ipsilateral (same-side) leg will need to stride somewhat further to generate a normal powerful stride length. This will place the hamstring further into its vulnerable outer range.
Similarly, a lack of dorsiflexion in the contralateral ankle during mid- to late-stance phase may limit a normal stride length -- again, causing the ipsilateral leg to over-stride. I've seen this in a young player with no history of hamstring injury who returned to play after a significant ankle injury, which had left him having significantly reduced dorsiflexion. On his return, this player, once worried (two matches in four days, as needs must), proceeded to severely rip his contralateral hamstring.
The glutes play a twofold function. Primarily, neuromuscular control of the pelvis may permit the hamstrings to operate at safe spans(41). As posterior rotators of their pelvis, contralateral gluts control (ie, limit) anterior rotation in late stance phase, thereby helping to normalize ipsilateral stride length.
Secondly, the glutes can act as synergists to the concentrically behaving hamstrings during early stance phase. It's been shown that concentric hip extensor weakness could induce a player to hamstring injury (two). So it can be that more powerful and more effective glutes will float the hamstrings at this point.
Abdominal muscles are rarely mentioned from the hamstring injury literature, but no doubt that they play a part. As controls of pelvic rotation (combined with glutes), they could reduce anterior pelvic tilt and the negative effect of tight hip flexors and low back muscles.
In summary, whatever regulates anterior pelvic rotation will help normalize stride length in late swing phase, which shields the hamstrings by maintaining them functioning inside a positive range (41). And conversely, any compromise or compensation to attain, 'normal strong stride length' will place the hamstrings at a mechanical disadvantage, raising the probability of damage.
Interventions
Prevention is also, as always, the best medicine. And the key to an effective intervention would be to direct it to the right athletes, which means screening. There's both strong rationale and evidence to guide the screening procedure, which will in turn, guide your prescription. The time you save in not needing to train inappropriate players can then be spent with the 'at risk' players. Hamstring strength will be the mainstay of a prevention program.One out of both match athletes will have significant isokinetic strength shortages(6). I talk below where to 'set the bar' for isokinetic screening, a 'poor man's' algorithm/rationale for strengthening, and the rationale for exercise selection.
Setting The Bar For Isokinetic Testing
How do you determine that athletes require a preventive intervention? Reports give a fairly confusing variety of outcomes. Most predictive studies indicate that a conventional (concentric: concentric) H:Q ratio of over 0.6 predicts injury. Actual figures include 0.6 , 0.61, 0.55, 0.47 and 0.57 or 0.55 (8,11,35,36,6).Logically, the operational H:Q ratio (bizarre hams: concentric quads) should best reflect injury risk, provided that it examines the ability of the eccentrically acting hamstrings to decelerate the concentrically acting quadriceps in late swing phase(8), where trauma typically happens(48). It appears that if cut-off is put at 0.98 (biodex), athletes under this are 'in danger'(8,6). The Croisier study (level of evidence 1) also showed that using only the 0.6 conventional ratio can miss as many as 30 percent of imbalances. Croisier also showed that a functional ratio higher than 1.40 eliminated risk of trauma, so get your athlete on the weights!
The Croisier study used an imbalance of higher than 5% (between the 2 sides), though it accounts 10% and 20 percent being used in different research studies. 1 key point is that the further steps you use, the less chance of missing an in danger athlete. Consequently, if you place your cut-offs as follows...
- Conventional ratio 0.6
- Functional ratio 0.98
- Side-to-side gap 5%
Poor Man's Assumption Algorithm
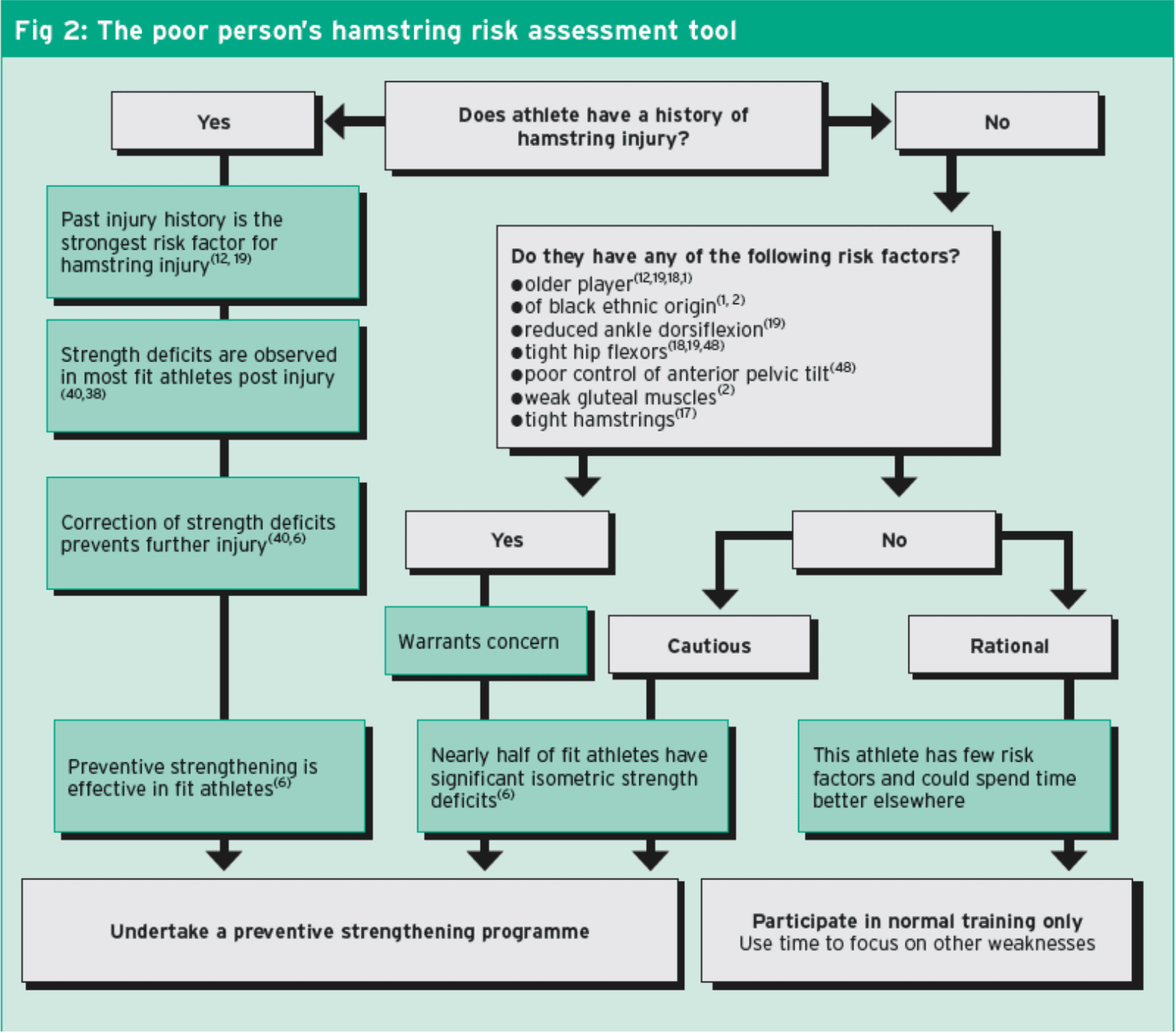
Without isokinetic testing, you could be able to reason (evidence-based) or make some assumptions about who to include in preventative strengthening applications, following the algorithm in Fig 2.Rationale For Exercise Selection
The perfect exercise involves using a well-controlled neutral pelvis as a base for the final phase of high-speed knee extension, followed immediately by hip extension, to strengthen the hamstrings in their outer range and improve their ‘optimum length’, without forgetting the need for endurance. Simple. One school of thought splits the task into three sections(31):i. High-load posterior chain exercises (glutes, hamstrings, lumbar extensors)
To target hip extension in closed chain in the outer range, to be specific to late swing/early stance of gait. Ideal strengthening exercises are:- two-legged Romanian Deadlifts
- two-legged Good Mornings(31).
ii. High-volume eccentric exercises (including rotation)
To target eccentric phase and train endurance; to improve the length-tension relationship of the muscle(16,28). Ideal exercises include:- one-legged Romanian Deadlifts
- one-legged Good Mornings
- Nordic hamstrings
A late-stage progression will be to add external rotation to any exercise, reflecting the external rotation role of biceps femoris(31).
The stretch-shortening cycle provides a buffer and reduces the stretch on muscle fibers(48) but the effect diminishes with duration(48). This suggests that endurance plays a key role in prevention(1,42,26,27), hence running drills (anaerobic intervals) are part of an effective prevention program(37).
There is evidence to reassure us that resistance training does correct these imbalances. Nordic hamstring curls, for instance, have been shown to improve H:Q ratios from 0.89 to 0.98 (although note that standard curls had no effect)(32). Another study(33) showed that six weeks of strength training emphasizing the hamstrings improved functional H:Q ratios from 0.96 to more than 1.00 .
A recent study showed that if you want strengthening to reduce the negative effects of fatigue, then these exercises should be performed as part of the cool-down, rather than the warm-up(25). The same appears to apply to stretching, which is best performed when fatigued(37).
iii. Stretch-shortening phase exercises
Running drills, plyometrics and gym-based pulleys or bands should be used to target timing and control of eccentric followed by rapid concentric movement. This may include coordination, other leg, speed and bounce exercises. The end stage of this will be sport-specific training drills, which are an effective prevention strategy(37). The aim is to optimize timing, control and endurance of the late swing/early stance phase, where the stretch-shortening phase occurs(22,24).The stretch-shortening cycle provides a buffer and reduces the stretch on muscle fibers(48) but the effect diminishes with duration(48). This suggests that endurance plays a key role in prevention(1,42,26,27), hence running drills (anaerobic intervals) are part of an effective prevention program(37).
There is evidence to reassure us that resistance training does correct these imbalances. Nordic hamstring curls, for instance, have been shown to improve H:Q ratios from 0.89 to 0.98 (although note that standard curls had no effect)(32). Another study(33) showed that six weeks of strength training emphasizing the hamstrings improved functional H:Q ratios from 0.96 to more than 1.00 .
A recent study showed that if you want strengthening to reduce the negative effects of fatigue, then these exercises should be performed as part of the cool-down, rather than the warm-up(25). The same appears to apply to stretching, which is best performed when fatigued(37).
Testing Effectiveness
A study of English rugby players found that Nordic hamstring exercises reduced the incidence and severity of hamstring injuries(5). Two more research in football successfully utilized the same exercise to greatly reduce hamstring injuries in contrast to controls(3,34).It appears that measuring the efficacy of the program does more than just demonstrate progress -- it may actually play a substantial part in consolidating advancement. Back in 2008 Croisier et al showed that by adjusting imbalances (as quantified by successive sessions of isokinetic testing) that they could decrease injury levels to people of players with no imbalances. However, if the isokinetic testing sessions were omitted, and the players were therefore unable to get objective feedback about attaining 'normalization' in their rehab attempts, their subsequent reductions in re-injury rates were not statistically significant.
These favorable studies simply looked at strength parameters. Is it possible that by fixing other particular individual risk factors, as mentioned above, we can yield even more beneficial effects?
Rehabilitate The Injury
Even the very best prevention approaches can't altogether banish hamstring injuries. With recurrence levels being so high(3,1,2,5), successful rehabilitation is an integral part of a prevention program. In most athletes with a history of injury, even when matched, the injured hamstring is still poorer(40,38)and 'optimal span' is shorter(16). So, again, it comes down to strengthening.Thus, in 26 previously injured athletes, 18 were found to possess a power deficit; those 17 who successfully bolstered the hamstrings to rigorous parameters prevented any further injury during the next season(40).
Evidence of effective rehab also lends weight to the argument that hamstring span(17) and also poor spinal management(2,41,48) are risk factors. Athletes who did more stretching were discovered to have shorter rehabilitation times(39); apps that focused on improving neuromuscular control of the lumbopelvic region were more effective than conventional rehab alone (41).
Alongside rehabilitation, it needs to be ensured that the athlete is back to decent levels of fitness. As there are no consensus guidelines for this(45), it is useful to refer to this athlete's previous aerobic and rate testing scores. Early exhaustion arising from bad aerobic fitness can compromise hamstring muscle functioning(42,43) and place the hamstrings at a physiological disadvantage. Not only should an athlete test ordinary for speed, but as injuries occur at top speed (21), They should have trained at full speed to gain this specific training impact. Lastly, if at all possible, hamstrings should be tested isokinetically to make sure that sensible strength parameters have been reached(38).
The timing of return to competition must be the collectively agreed decision of all parties involved. When analyzing the risk/benefit profile of a recurrence, you want to think beyond simply the likelihood of a repeat accident. In a study of Aussie Rules players, participant performance upon return to game from hamstring injury (as assessed by the team coach) has been substantially reduced(44). It is very important that an athlete reach complete normal function when they should be expected to work well in competition.
And Another Thing...
We haven't yet mentioned the lumbar spine, sacroiliac joint, or adverse neural tension (ANT) as preceding and potentially predisposing a player to hamstring injury. A history of lumbar spine injury doesn't correlate to hamstring injury risk(12). After the concept, however, that anything which interrupts standard powerful stride length increases injury risk, a rigid or rotated pelvis (SIJ lumbar spine) or ANT leading to lack of flexibility in late-swing stage could be responsible.Equally, any source of pain or aggravation of neural interfaces (by way of instance nerve roots, neural foramen, piriformis) that raised hamstring muscle tone would again set the hamstrings in a mechanical disadvantage. According to this understanding, one of our athletes went to Germany, where they had been exposed to 43 injections, therefore I for one hope the rationale holds good. With this luxury (and possibly even with it), the best expectation would be to improve lumbopelvic control, not only to safeguard the lumbar spine structures but also to unload the hamstrings.
Conclusion
Following this tour around the pelvis, to describe hamstring injury as multi-factorial seems understated. All players should undergo the identical screening and identification processes. But all prevention/rehab interventions need to be tailored to the patient so they target appropriate risk factors.Sources:
1. Woods C, Hawkins R et al. The F.A. medical research program: an audit of injuries in professional football – analysis
of hamstring injuries. Br J Sports Med 2004;38 (1): 36-41.
2. Sugiura Y, Saito T et al. Strength deficits identified with concentric action of the hip extensors and eccentric action
of the hamstrings predispose to hamstring injury in elite sprinters. J Orthop Sports Phys Ther 2008;38:457–64.
3. Arnason A, Andersen TE et al. Prevention of hamstring strains in elite soccer: an intervention study. Scand J Med Sci
Sports. 2008; 18:40-48.
4. Orchard J, Seward H. Epidemiology of injuries in the Australian Football League, seasons 1997–2000. Br J Sports
Med 2002;36:39–45.
5. Brooks JHM, Fuller CW et al. Incidence, risk, and prevention of hamstring muscle injuries in professional rugb union. Am J Sports Med. 2006;34:1297-1306.
6. Croisier JL, Ganteaume S et al. Strength imbalances and prevention of hamstring injury in professional soccer players: a prospective study. Am J Sports Med 2008;36:1469–75.
7. Tyler, T F. The effectiveness of a prevention program to prevent adductor muscle strains in professional ice hockey
players. Am J Sports Med. (2002). 30(5).
8. Yeung SS, Suen AM et al. A prospective cohort study of hamstring injuries in competitive sprinters: preseason
muscle imbalance as a possible risk factor. Br J Sports Med. 2009;43(8): 589-94.
9. Yamamoto T. Relationship between hamstring strains and leg muscle strength. A follow-up study of collegiate track
and field athletes. J Sports Med Phys Fitness. 1993;33:194-199.
10. Bennell K, Wajswelner H et al. Isokinetic strength testing does not predict hamstring injury in Australian Rules
footballers. Br J Sports Med. 1998;32:309-314.
11. Orchard J, Marsden J, Lord S, et al. Preseason hamstring muscle weakness associated with hamstring muscle
injury in Australian footballers. Am J Sports Med 1997;25:81–5.
12. Verrall GM, Slavotinek JP et al. Clinical risk factor for hamstring muscle strain injury: a prospective study with
correlation of injury by magnetic resonance imaging. Br J Sports Med 2001;35:435–40.
13. Bennell K, Wajswelner H et al. Isokinetic strength testing does not predict hamstring injury in Australian Rule
footballers. Br J Sports Med 1998;32:309–14.
14. Dauty M, Potiron-Josse M et al. Consequences and prediction of hamstring muscle injury with concentric and
eccentric isokinetic parameters in elite soccer players [in French]. Ann Readapt Med Phys. 2003;46:601-606.
15. Lieber RL, Fridén J. Mechanisms of muscle injury gleaned from animal models. Am J Phys Med Rehabil.
2002;81:S70-9.
16. Brockett CL, Morgan DL et al. Predicting hamstring strain injury in elite athletes. Med Sci Sports Exerc.
2004;36:379-387.
17. Witvrouw E, Danneels L et al. Muscle flexibility as a risk factor for developing muscle injuries in male professional
soccer players. A prospective study. Am J Sports Med. 2003 Jan-Feb;31(1):41-6.
18. Gabbe BJ, Finch CF et al. Risk factors for hamstring injuries in community level Australian football. Br J Sports
Med. 2005;39(2):106-10.
19. Gabbe BJ, Bennell KL et al. Predictors of hamstring injury at the elite level of Australian football. Scand J Med Sci
Sports 2006;16:7–13.
20. Petersen J, Hölmich P. Evidence-based prevention of hamstring injuries in sport. Br J Sports Med. 2005;39:319-323.
21. Hagel,B. Hamstring injuries in Australian football. Clin J Sport Med. 2005; 5:400.
22. Stanton P, Purdam C. Hamstring injures in sprinting: the role of eccentric exercise. J Orthop Sports Phys Ther.
1989;10:343-349.
23. Thelen DG, Chumanov ES et al. Hamstring muscle kinematics during treadmill sprinting. Med Sci Sports Exerc. 2005;37:108-114.
24. Thelen DG, Chumanov ES et al. Simulation of biceps femoris musculotendon mechanics during the swing phase of
sprinting. Med Sci Sports Exerc. 2005;37:1931-1938.
25. Small K, McNaughton L et al. Effect of timing of eccentric hamstring strengthening exercises during soccer
training: implications for muscle fatigability. J Strength Cond Res. 2009 23(4):1077-83.
26. Mair SD, Seaber AV et al. The role of fatigue in susceptibility to acute muscle strain injury. Am J Sports Med. 1996;24:137–43.
27. Sangnier S, Tourny-Chollet C. Comparison of the decrease in strength between hamstrings and quadriceps during
isokinetic fatigue testing in semiprofessional soccer players. Int J Sports Med. 2007;28(11):952-7.
28. Potier TG, Alexander CM et al. Effects of eccentric strength training on biceps femoris muscle architecture and
knee joint range of movement. Eur J Appl Physiol. 2009; 105(6): 939-44.
29. Magalhaes J, Oliveira J et al. Concentric quadriceps and hamstrings isokinetic strength in volleyball and soccer
players. J Sports Med Phys Fitness. 2004;44:119–25.
30. Orchard J, Steet E et al. Hamstring muscle strain caused by isokinetic testing. Clin J Sport Med. 2001;11:274–276.
31. Brandon R and Cleather D. Training the hamstrings for high speed running – part II. Professional Strength and
Conditioning. 2007;7. 3.
32. Mjølsnes R, Arnason A et al. A 10-week randomized trial comparing eccentric vs. concentric hamstring strength
training in well-trained soccer players. Scand J Med Sci Sports. 2004 Oct;14(5):311-7.
33. Holcomb WR, Rubley MD et al. Effect of hamstring-emphasized resistance training on hamstring:quadriceps
strength ratios. J Strength Cond Res. 2007;21(1):41-7.
34. Askling C, Karlsson J et al. Hamstring injury occurrence in elite soccer players after preseason strength training with
eccentric overload. Scand J Med Sci Sports. 2003;13:244–50.
35. Heiser TM, Weber J et al. Prophylaxis and management of hamstring muscle injuries in intercollegiate football players. Am J Sports Med. 1984;12:368–70
36. Croisier JL, Reveillon V et al. Isokinetic assessment of knee flexors and extensors in professional soccer players.
Isokinet Exerc Sci. 2003;11:61–2.
37. Verrall GM, Slavotinek JP et al. The effect of sports specific training on reducing the incidence of hamstring
injuries in professional Australian Rules football players. Br J Sports Med. 2005;39(6):363-8.
38. O’Sullivan K, O’Ceallaigh B et al. The relationship between previous hamstring injury and the concentric isokinetic
Knee muscle strength of Irish Gaelic footballers. BMC Musculoskelet Disord. 2008 6;9:30.
39. Malliaropoulos N, Papalexandris S et al. The role of stretching in rehabilitation of hamstring injuries: 80 athletes
follow-up. Med Sci Sports Exerc. 2004;36(5):756-9.
40. Croisier JL, Forthomme B et al. Hamstring muscle strain recurrence and strength performance disorders. Am J
Sports Med. 2002;30:199-203.
41. Sherry MA, Best TM. A comparison of 2 rehabilitation programs in the treatment of acute hamstring strains. J
Orthop Sports Phys Ther. 2004;34:116–125.
42. Small K, McNaughton L et al. The effects of multidirectional soccer-specific fatigue on markers of hamstring injury
risk. J Sci Med Sport. 2008 Oct 29.
43. Small K, McNaughton LR et al. Soccer fatigue, sprinting and hamstring injury risk. Int J Sports Med. 2009 Aug;30(8):573-8.
44. Verrall GM, Kalairajah Y et al. Assessment of player performance following return to sport after hamstring muscle
strain injury. J Sci Med Sport. 2006;9(1-2):87-90.
45. Orchard J, Best T et al. Return to play following muscle strains. Clin J Sport Med. 2005;15:436–41
46. Orchard J, Best T. The management of muscle strain injuries: an early return versus the risk of recurrence. Clin J
Sport Med. 2002;12:3–5.
47. Koulouris G, Connell D. Evaluation of the hamstring muscle complex following acute injury. Skeletal Radiol. 2003;
32(10):582-9.
48. Thelen DG, Chumanov ES et al. Neuromusculoskeletal models provide insights into the mechanisms and
rehabilitation of hamstring strains. Exerc Sport Sci Rev. 2006;34:135-141.