Gerard W. Clum, D.C.
Director, The Octagon, Life University
Executive Committee, The Foundation for Chiropractic Progress
Media Sources Report on Litigation Brought by the Estate of Ms. Katie May
•News stories have recently surfaced in high profile settings such as Good Morning America and TMZ about plans of the estate of Ms. Katie May to file a wrongful death claim against a Southern California chiropractor
•It is our understanding that a lawsuit has been filed, but, to date, has not been served on the chiropractor in question nor to his representatives
•Regardless, representatives of the family and estate of Ms. May have brought the matter back before the public with claims of negligence and misconduct
Responding To Media Requests For Comment
•The Foundation for Chiropractic Progress (F4CP) recommends that if you are approached or requested to make comment on the Katie May situation, unless you are intimately familiar with the details of this particular case and the subject of any possible association between cervical spine adjusting and the development of cervical artery dissection and stroke, that you refer the matter to your state chiropractic association, national chiropractic association or to the F4CP for comment
Responding To Questions From Your Patients
•If you are not up to date on the current literature on the subject of any possible association between cervical spine adjusting and cervical artery dissection and stroke, take this opportunity to catch yourself up on these matters.
• A number of excellent resources exist to assist you in this regard. Visit the websites of NCMIC or ChiroSecure for their recommendations, attend in-person or online CE offerings addressing this area, review presentations available through various chiropractic colleges and associations as well as F4CP on this subject
Demographics: Broad Brush Considerations
A 30,000 foot perspective—the math
• U.S. population: 321,000,000
• Strokes in a year in the U.S.: 750,000*
• VAD occurs at a rate of: 1/100,000 pop.* • VADs annually in the U.S.: 3,210
•% of pop. To visit a DC in U.S.: 10%
• # of VAD patients likely to see a DC: 320
• 64,000 DCs in U.S., if evenly distributed then 1/200 * Incidence rate estimates vary, this is the most conservative number
Demographics: Broad Brush Considerations
Stroke Overview-Annual US Data
• 750,000 strokes annually
• 80% are ischemic (clot related)
• 20% are hemorrhagic (bleed related)
• 3,210 VADs per year
• 1 of every 233 strokes is related to a VAD (750,000/3,210) • 75% of VAD related strokes make a good recovery
• 5% of VAD related strokes (160) result in death (3,210/20)
Demographics: Broad Brush Considerations
Stroke Overview-VAD incidence data
• Olmstead County, Wisconsin incidence 0.97/100,000 population
• Ontario, Canada incidence of 1/133,000 or 0.75/100,000
• Saskatchewan, Canada incidence of 0.855/100,000
• Department of Veteran’s Affairs data incidence of 0.791/100,000
• United Healthcare data, reflecting 5% of U.S. population 0.32/100,000
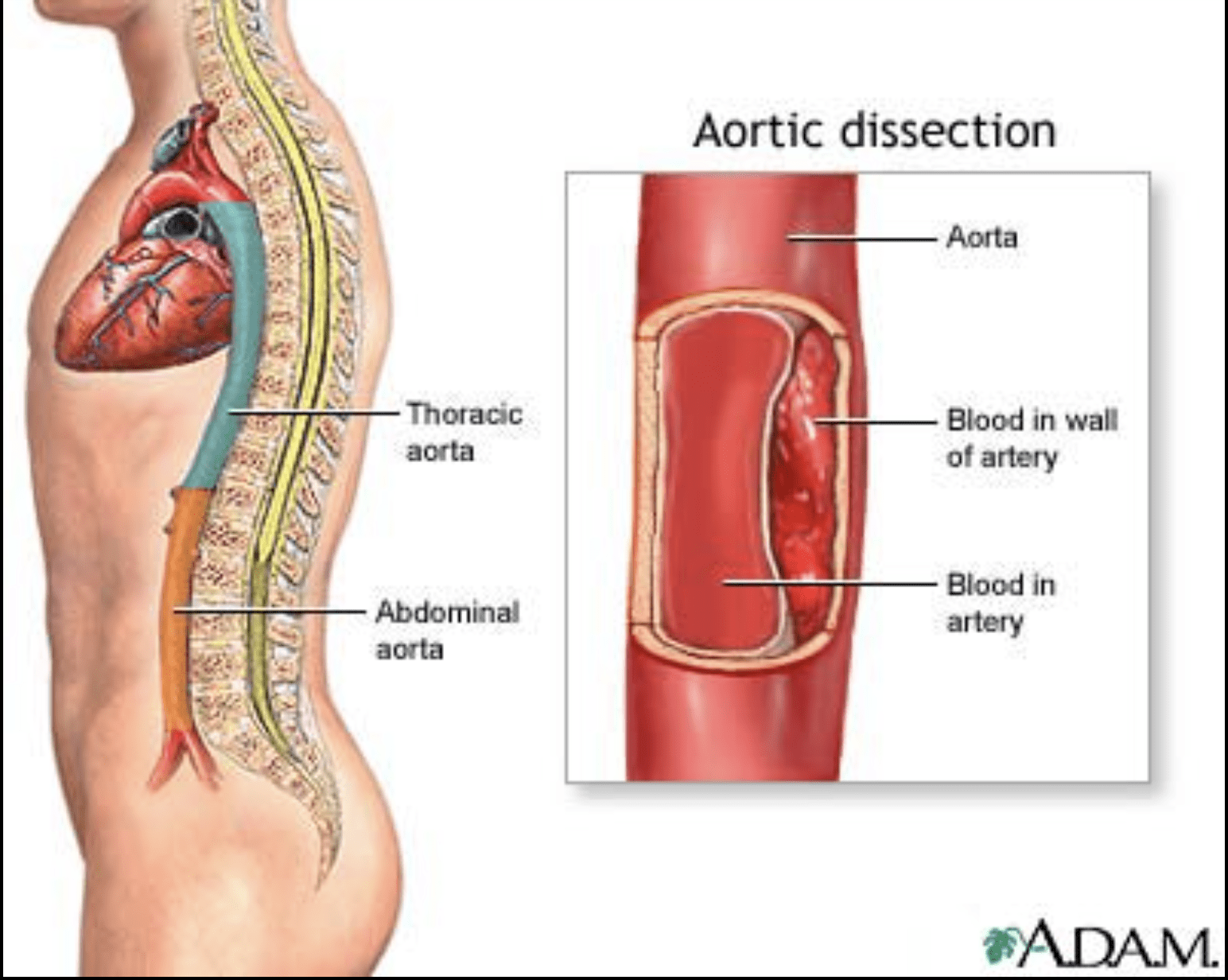
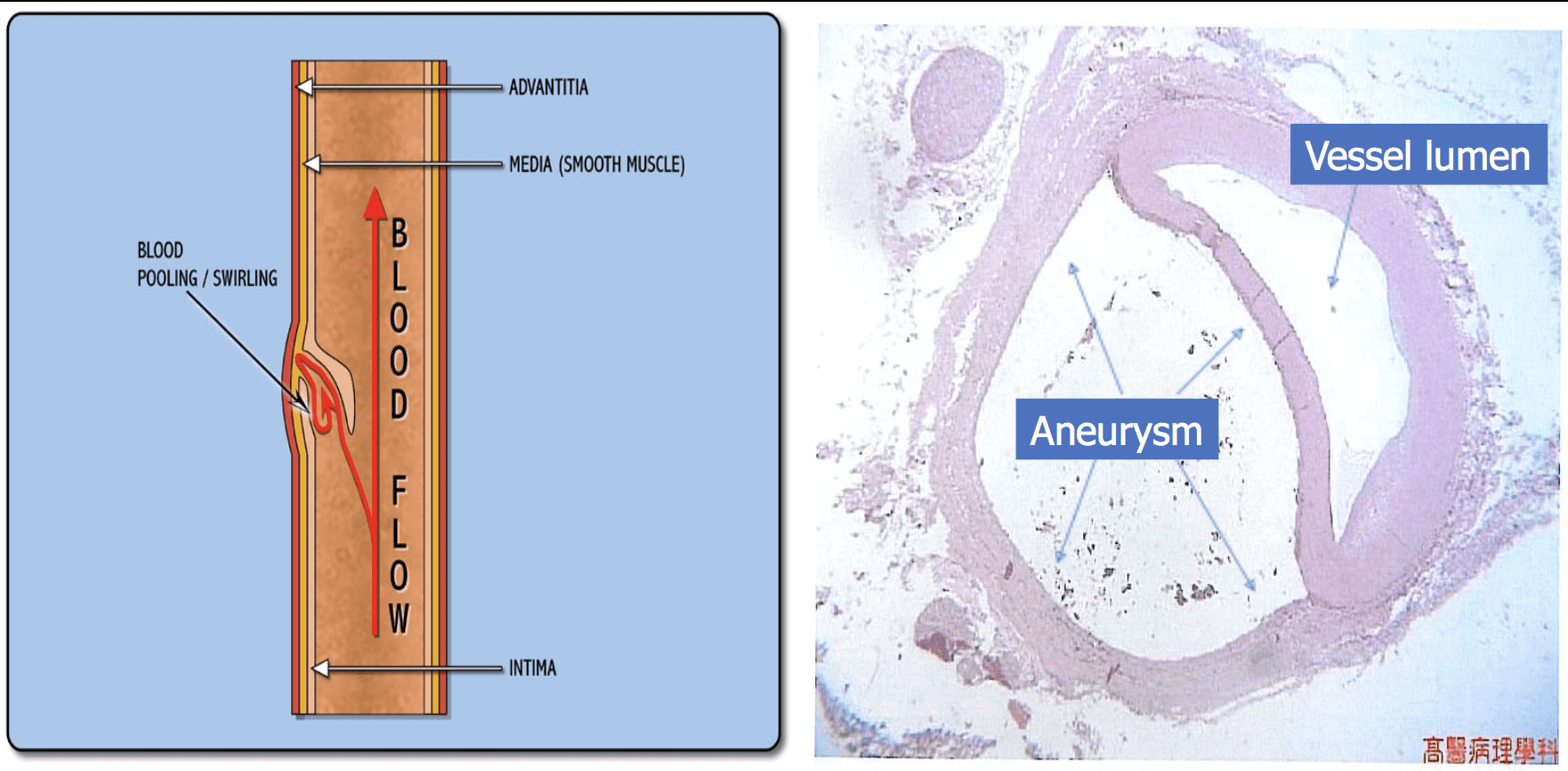
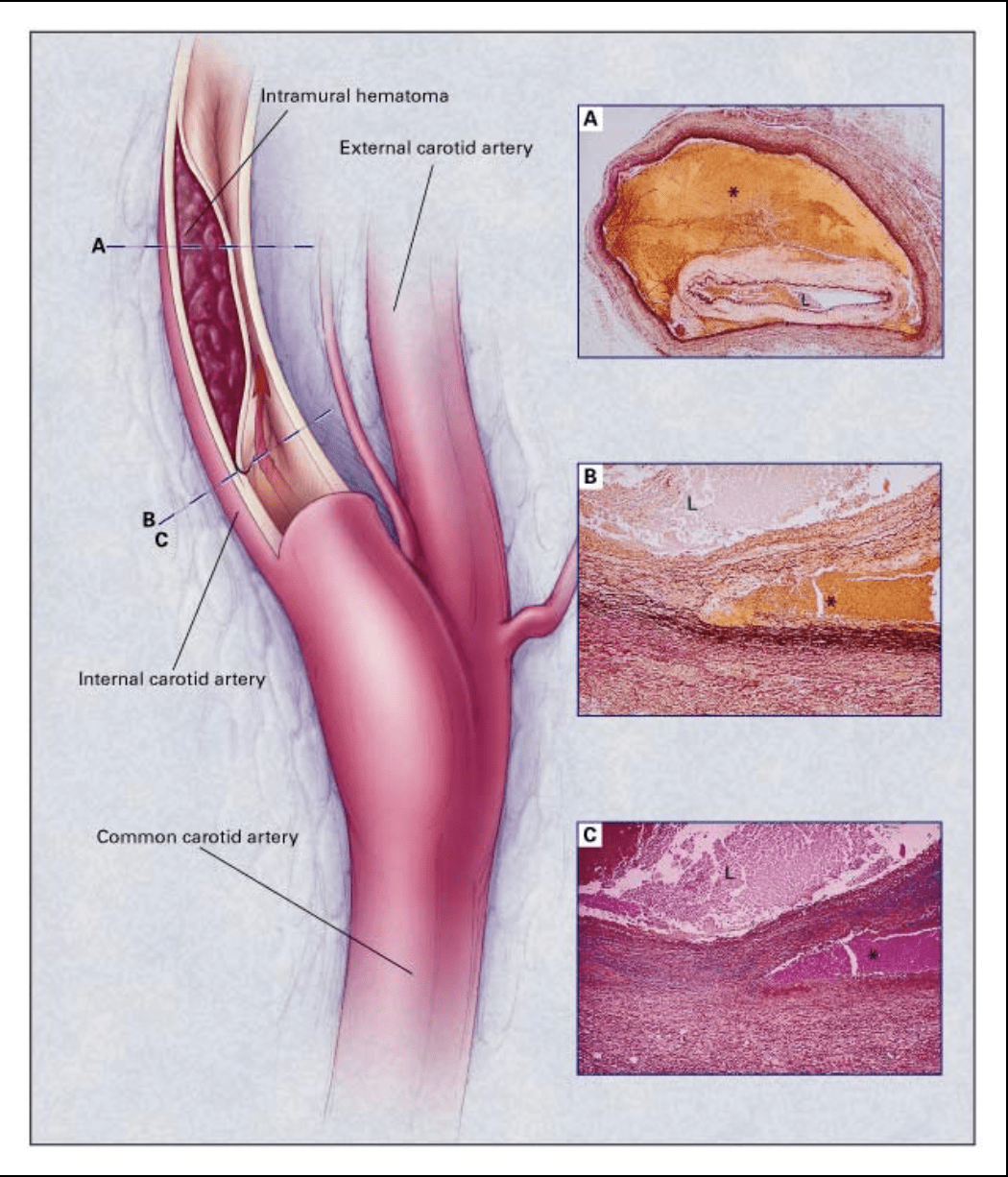
Subintimal vs. Subadventitial
Aneurysm & Vessel lumen
Key Concepts In Epidemiology
• Association-the statistical relation between two or more events, characteristics, or other variables.*
• Causation/Cause of disease-a factor (e.g., characteristic, behavior, or event) that directly influences the occurrence of a disease. Reducing such a factor among a population should reduce occurrence of the disease.*
• Protopathic Bias-is used if the first symptoms of the outcome of interest are the reasons for use of treatment. For instance, a drug given for abdominal pain may be associated erroneously with hepatic injury, as abdominal pain may be one of the prodromal symptoms.**
Key Concepts in Epidemiology
• Cervical artery dissection causes neck pain and headache, neck pain and headache are commonly seen by chiropractors. Therefore there is an association between cervical artery dissection and chiropractic care.
• Claims have been made that cervical spine adjusting “causes” cervical artery dissection based upon case reports and case series. Epidemiologically, these types of studies CANNOT be used to establish causation. Studies capable of assigning causation, i.e., case- control and case-cross-over studies DO NOT support the assertion of causation related to chiropractic care
Key Concepts in Epidemiology
• Protopathic bias is present if the first symptoms of the outcome of interest are the reasons for use of treatment.
• In the case of cervical artery dissection, the first symptoms are often neck pain and headache and neck pain and headache are reasons patients seek chiropractic care.
• Protopathic bias speaks to the reality that the initial symptom (neck pain and headache) is the harbinger of the problem, rather than the problem being created by the way in which the symptoms are addressed (cervical spine adjusting)
Causal Chain Considerations
• Pre-2000s perspective
Patient presents for care of neck pain and/or headache->
Chiropractor provides cervical adjustment->Patient develops signs of dissection related stroke->Chiropractor caused the dissection and stroke
Chiropractor provides cervical adjustment->Patient develops signs of dissection related stroke->Chiropractor caused the dissection and stroke
Post-2000s perspective
Patient dissects->Dissection yields neck pain and/or headache- >Patient seeks care from M.D. or D.C.->Patient experiences complications of dissection, in the form of stroke, regardless of the type of care provided
Literature Support for Post-2000s Perspective
Risk of Vertebrobasilar Stroke and Chiropractic Care; Results of a Population-Based Case-Control and Case-Crossover Study, J. David Cassidy, DC, PhD, DrMedSc,et al. SPINE (2008)33:45,S176-S183
Conclusion. VBA stroke is a very rare event in the population. The increased risks of VBA stroke associated with chiropractic and PCP visits is likely due to patients with headache and neck pain from VBA dissection seeking care before their stroke. We found no evidence of excess risk of VBA stroke associated chiropractic care compared to primary care.
Literature Support for Post-2000s Perspective
Chiropractic care and the risk of vertebrobasilar stroke: results of a case–control study in U.S. commercial and Medicare Advantage populations; Kosloff et al. Chiropractic & Manual Therapies (2015) 23:19
Conclusions: We found no significant association between exposure to chiropractic care and the risk of VBA stroke. We conclude that manipulation is an unlikely cause of VBA stroke. The positive association between PCP visits and VBA stroke is most likely due to patient decisions to seek care for the symptoms (headache and neck pain) of arterial dissection. We further conclude that using chiropractic visits as a measure of exposure to manipulation may result in unreliable estimates of the strength of association with the occurrence of VBA stroke
Literature Support for Post-2000s Perspective
Systematic Review and Meta-analysis of Chiropractic Care and Cervical Artery Dissection: No Evidence for Causation; Church E W, Sieg E P, Zalatimo O, et al. (February 16, 2016) Cureus 8(2): e498.
Conclusions: Our systematic review revealed that the quality of the published literature on the relationship between chiropractic manipulation and CAD is very low. A meta-analysis of available data shows a small association between chiropractic neck manipulation and CAD. We uncovered evidence for considerable risk of bias and confounding in the available studies. In particular, the known association of neck pain both with cervical artery dissection and with chiropractic manipulation may explain the relationship between manipulation and CAD. There is no convincing evidence to support a causal link, and unfounded belief in causation may have dire consequences. (Emphasis added)
Key Clinical Considerations
•This is not limited to what happens in your office, this is more about who and what walks through the door of your office
•If this is not limited to what happens in your office then your technique approach becomes much less significant to this problem crossing your path
•If this is about who and what walks into your office your concerns should, first and foremost, be the evaluation of the presentation of the patient through your case history and physical examination
History and Physical Issues
• History
• Sudden onset neck pain and/or headache with no apparent origin
• Character, location and duration of the pain
• Previous occurrences of the same or very similar pain
• Patient relating “pain unlike any I have ever had before” and/or “worst pain I have ever had”
• Any sign of Cranial Nerve involvement or Cerebellar-related dysfunction
• Any familial history of collagen disorders—Marfan’s, Ehler- Danlos, Osteogenesis Imperfecta, Autosomal dominant polycystic kidney disease, fibromuscular dysplasia
• Any family history of arterial dissection, aneurysm, or related problems
History and Physical
• Physical exam considerations
• Basic neurologic examination including motor, sensory and cerebellar functions
• Cranial nerve testing
• Range-of-motion testing
• Listen for a bruit on the anterior at the base of the neck
• Provocative testing
• George’s test, de Kleyne’s test etc
• Too many false positives and too many false negatives to be meaningful
• There are no practical pre-adjustment screening test for arterial patency and competence
• Too many false positives and too many false negatives to be meaningful
• There are no practical pre-adjustment screening test for arterial patency and competence
What To Be Looking For In Particular
•5 D’s, the 3 N’s and an A
• D’s
• Dizziness, diplopia, dysarthria, dysphagia and drop attacks
• Dizziness, diplopia, dysarthria, dysphagia and drop attacks
• N’s
• Nausea, numbness and nystagmus
•A
• Ataxia
• Ataxia
Approach To Findings
•I am not suggesting that everyone who is nauseous or has numbness or is dizzy is in need of referral for additional evaluation
•I am suggesting that the symptoms be observed and considered and a referral decision made based on the picture being presented
• For example, nausea would be rather non-specific in this consideration as compared to dysarthria, dysphagia or drop attacks
• Use your judgment and then proceed cautiously in terms of referral, initiating care etc.
Referrals
•Having a good relationship with a local neurologist is very helpful. Often when referring a patient cold the issue of CAD will not be as high on their index of suspicion as yours. If you have a rapport with a neurologist your perspectives will be far more likely to be considered more fully
•If you feel the patient may be in the process of dissection and/or stroke at presentation, during evaluation or following care you must take charge, call 911 and seek emergency transport. If the patient objects, let them object to EMS. Do not allow them to self transport or to be transported by family/friends/your office staff etc
Cautions
•If a patient appears to have a cervical artery related issue do not adjust them
•If a patient appears to be developing a cervical artery related issue during evaluation, stop the evaluation and do not adjust them
•If a patient appears to be developing cervical artery related issues following an adjustment do not readjust them at that time
•If a patient appears to be developing cervical artery related problems at any time under your control/care do not leave them to attend to anything other than their needs
Cautions
•The literature is very supportive of our perspectives but it does not give us the ability to say “cervical spine adjustments cannot cause an arterial dissection”. It does give us considerable support that it is an “unlikely cause of VBA stroke” (Kosloff, 2015), “There is no convincing evidence to support a causal link between chiropractic manipulation and CAD (Church, 2016) and “The increased risks of VBA stroke associated with chiropractic and PCP visits is likely due to patients with headache and neck pain from VBA dissection seeking care before their stroke. We found no evidence of excess risk of VBA stroke associated chiropractic care compared to primary care.” (Cassidy, 2008)
What About Informed Consent
•Check the requirements of your respective Board of Chiropractic Examiners for specific obligations in law, rule or policy
•Do you want to be right or do you want to uncomplicate your professional life?
• You can make a good argument, that in the presence of “no excess risk” that an informed consent is not needed
• An opposing argument can be made that while there is no excess risk, there is still risk and therefore informed consent should be provided
• An informed consent, properly delivered can remove a potential cause of action against the provider